Washington People: Gregory Zipfel
Neurosurgeon dedicated to making surgeries smaller, less invasive
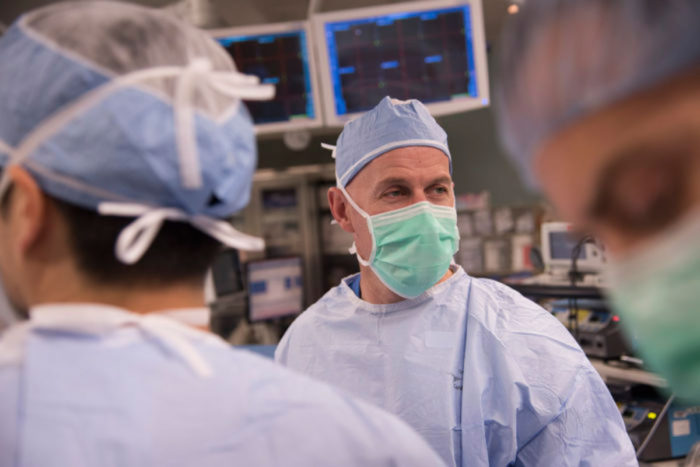 Robert Boston
Robert BostonGreg Zipfel, MD, seen here during a neurosurgery at Barnes-Jewish Hospital, has dedicated his career to treating diseases of the brain and nervous system, particularly abnormalities of the blood vessels leading to and inside the brain. His goal is to make neurosurgeries smaller, less invasive and all-around easier on patients.
“Seeing a human brain for the first time as a medical student, and seeing that it has a pulse and can move and is active, is awe-inspiring,” said Gregory Zipfel, MD, a professor of neurological surgery and neurology at Washington University School of Medicine in St. Louis. “The brain is uniquely beautiful.”
In the decades since, some of the awe has worn off but none of the inspiration. Zipfel, who describes his first neurosurgical procedure as “exhilarating,” has dedicated his career to treating diseases of the brain and nervous system, particularly abnormalities of the blood vessels leading to and inside the brain.
“It was the intensity of neurosurgery that drew me to this field,” Zipfel said. “There are lots of careers where you can contribute to society in a meaningful way, but I would argue that helping an individual, a whole family, through an illness is hard to beat.”
 Robert Boston
Robert BostonZipfel received his bachelor’s degree from the University of Illinois in 1991 and his medical degree from Northwestern in 1995. He then trained as a neurosurgery resident at the University of Florida before joining the faculty at Washington University in 2004.
“When he first came to WashU, I asked him to help me on a risky project,” said David Brody, MD, PhD, a professor of neurology. “It was a lot of work, and it could have yielded nothing. A lot of people wouldn’t have taken on a project like that, especially since it required him to come in in the middle of the night, but he agreed right away and threw himself into it. And it worked out fantastically well. That was my first experience with Greg, and I was just so impressed with his dedication and willingness to take risks.”
The study, which showed that levels of the Alzheimer’s disease-associated protein amyloid beta were associated with neuronal activity, was published in Science in 2008.
Dedication and willingness to take risks sum up Zipfel’s approach to his work. His goal is to make neurosurgeries smaller, less invasive and all-around easier on patients so they can get back to their regular lives in days or weeks rather than months.
To this end, he has been working to use an endoscope – a thin, flexible tube with a tiny camera and light at the end – to provide images so doctors can perform surgeries such as removing tumors through a patient’s nose. The scope is inserted through the nostril and threaded through the back of the nose to the tumor site. These techniques allow a patient to recover more quickly without a disfiguring scar.
Other surgeries, such as those to repair brain aneurysms – weak areas of blood vessels that balloon out and can rupture easily – can’t be performed through the nose. Traditionally, repairing brain aneurysms has required craniotomies, in which a piece of the skull is temporarily removed to give surgeons access to the brain. Zipfel is working on techniques to replace craniotomies with mini-craniotomies, in which surgeons repair blood vessels through small holes drilled into the skull.
“It was clear from day one that he was really serious about being a great neurosurgeon,” said Arthur Day, MD, who mentored Zipfel during his neurosurgery residency. “He always wanted to make sure that everything he was doing would be done right.”
Zipfel’s drive to excel makes him well-suited for the delicate, high-stakes world of neurosurgery, where the slightest imprecision could have devastating consequences for the patient.
“The patient who sticks with me is a 14-year-old boy with a large, complex aneurysm,” said Zipfel, who treated the boy by clipping the blood vessel at the site of the aneurysm and routing the blood flow around it. “Recently, he started college. It’s really thrilling to see a boy go through a major illness and prosper in the long-term.”
Outside of neurosurgery, sports drive Zipfel.
“I don’t have a lot of hobbies, but whatever I’m involved in, I tend to be focused on doing it well,” Zipfel said. When he was a medical resident, that involved playing a lot of baseball.
“He was a powerful athlete,” recalled Day. “He could hit a baseball a long, long ways.”
These days, Zipfel spends his free time with his wife and three young children – attending his daughter’s dance recitals and going out to dinner with his wife, Washington University pediatrician Mary Jo Hernandez, MD. He’s still a huge sports fan, though.
“One of his favorite things to do at scientific conferences is to go to his room, put sports on the TV and write a grant,” Brody said. “That’s his idea of a good time. But it works for him. He gets the grants.”
Zipfel’s sport of choice these days is golf, which he frequently plays with his 9-year-old son. “My son is very much like me,” Zipfel said with a laugh. “A little compulsive.”







