Treating prostate cancer with precision
A new needle-based treatment for less aggressive forms of prostate cancer is now available
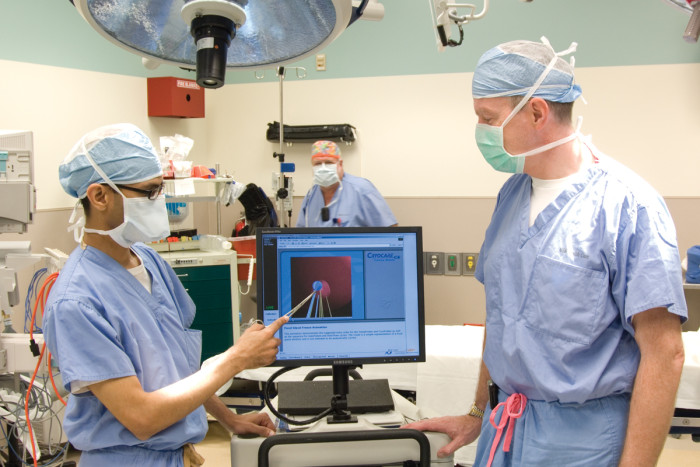 Robert Boston
Robert BostonSam Bhayani, MD, left, and Robert Figenshau, MD, use special software to plan placement of cryoneedles directly into the prostate to kill the prostate cancer.
The treatment, called focal needle ablation, makes use of a needle that can freeze (cryoablation) or use heat (radiofrequency ablation) to destroy cancer cells.
In the past, when a biopsy—the standard diagnostic procedure for the past 20 years—detected a small amount of prostate cancer, it wasn’t known whether the cancer was small or whether the biopsy had grazed the side of a large tumor. Erring on the side of caution, urologic surgeons would make a large incision in the abdomen to remove the entire prostate. As treatment options advanced, the Alvin J. Siteman Cancer Center at Barnes-Jewish Hospital and Washington University School of Medicine was among the first centers in the United States to perform laparoscopic, nerve-sparing radical prostatectomy for most patients with prostate cancer. During the past decade, treatment of small cancers has taken another step forward, with urologists using needle ablations to freeze and kill cancerous areas in the prostate.
“We’ve come to recognize that radical prostatectomy or radiation to treat the entire prostate can be overtreatment. And overtreatment results in too many side effects and unnecessary costs,” says Gerald Andriole Jr., MD, chief of the Division of Urologic Surgery. “If we can tailor the treatment to the man’s individual cancer, he will benefit, and the treatment will be more efficient.”
Cryoablation: The “male lumpectomy”
Washington University urologic surgeons at Barnes-Jewish Hospital first used cryoablation as an investigational treatment and now use it in about 10 percent of prostate cancer cases. They also use cryoablation for focal treatment of kidney and liver cancer.
For prostate cancers, the treatment process begins with a biopsy and ultrasound to determine the size and location of the cancer. Optimally, magnetic resonance imaging (MRI) is used to confirm the cancer’s location and determine that it truly is localized.
During a cryoablation procedure, the urologic surgeon, using ultrasound guidance, inserts one or two cryoneedles below the scrotum and into the prostate. The needles freeze small pear-shaped areas that include the cancerous parts of the gland. The treatment is performed as an outpatient procedure, and most patients are well enough to return to work the next day.
“In the last few years, our targeting has improved as imaging technology has advanced,” says urologic surgeon Sam Bhayani, MD. “We work closely with radiologists at Washington University’s Mallinckrodt Institute of Radiology, who use advanced 3 Tesla MRI and ultrasound technology.”
The procedure is known as male lumpectomy because it preserves a major part of the prostate, just as a lumpectomy to treat breast cancer preserves most of the breast tissue. Urologic surgeons take great care to avoid the rectum and the nerves needed for erections, which are located just outside the prostate. “You need very detailed, continuous monitoring when you are performing cryoablation,” says Andriole.
Vascular-targeted photodynamic therapy
Washington University urologists have completed a clinical trial to evaluate what may be the next advancement in focal ablation: vascular-targeted photodynamic therapy (VTP).
In VTP, an intravenously injected drug adheres to the capillaries that provide blood supply to tumors. These capillaries, which help the cancer grow, differ from blood vessels associated with healthy tissues. Laser energy released from a fiber placed next to the cancer-supplying capillaries blocks the blood vessels, which interrupts blood flow to the cancer and kills tumor tissue.
“Cancers have a growth pattern that’s a lot like a tree,” says Andriole. “There’s a good deal of normal prostate tissue in between the tentacles and branches of the cancer. When you perform cryoablation, you’re making a pear-shaped ice ball that kills everything inside the ball—cancerous and normal tissue. There are likely more side effects with cryoblation than with VPT, in which you’re more selectively killing the cancer.”
The Food and Drug Administration will review data from the VTP clinical trial at Washington University and elsewhere. If the therapy is approved, it will be offered at Siteman Cancer Center.
Identifying aggressive cancers
To determine the best treatment options, Washington University urologists are investigating new ways to determine which prostate cancers are slow-growing and which are more aggressive.
Pathologists have traditionally relied on Gleason scoring to measure cancer aggressiveness. Looking under a microscope at multiple biopsy specimens taken from different areas of a patient’s prostate, they categorize tumor patterns on a scale of 1 to 5, with 5 being the most aggressive. The two top scores are added, with a final range of 2 to 10.
But Gleason scores aren’t always accurate, so Andriole and a team of scientists at The Elizabeth H. and James S. McDonnell III Genome Institute at Washington University are looking at the genetic makeup of prostate cancers.
“When we remove a cancerous prostate, there are, on average, at least five separate cancers in it,” Andriole says. “Are the genes that these different cancers express the same or different? If they are different, how can we use those differences to more precisely characterize the aggressiveness of a man’s cancer?”







