Surgery for early prostate cancer may not save lives
Most men just as likely to survive with limited or no treatment
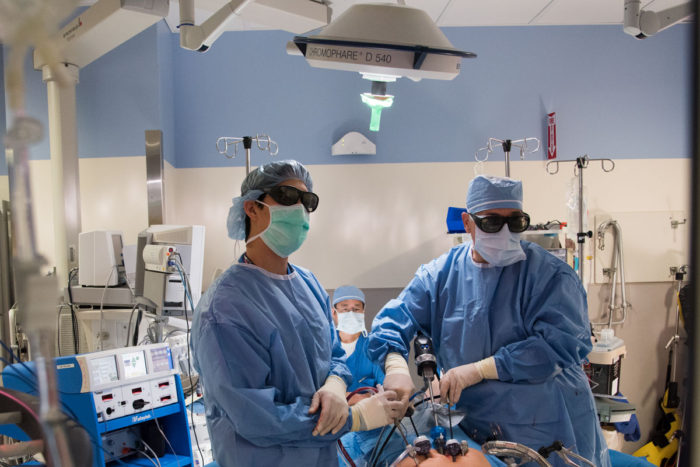 Robert Boston
Robert BostonGerald L. Andriole, MD, (right) director of Washington University's Division of Urologic Surgery, performs surgery on a patient with prostate cancer. New research provides further evidence that surgery is unnecessary for early-stage prostate cancer, although some men whose disease is further along may benefit.
A major 20-year study provides further evidence that prostate cancer surgery offers negligible benefits to many men with early-stage disease. In such men, who account for most cases of newly diagnosed prostate cancer, surgery did not prolong life and often caused serious complications such as infection, urinary incontinence and erectile dysfunction.
The study, by a national research team including Washington University School of Medicine in St. Louis, was led by the Minneapolis Veterans Administration Health Care System. It is published July 13 in The New England Journal of Medicine.
In men with early prostate cancer, the study compared surgery with observation. With the latter, men only were treated if they developed bothersome symptoms, such as urinary difficulty or bone pain. Such symptoms may indicate progression of the cancer. Many men in the observation group received no treatment at all because early-stage prostate cancer often grows slowly and rarely causes symptoms.
“The findings will go a long way in helping to improve prostate cancer care,” said co-author Gerald L. Andriole, MD, director of Washington University’s Division of Urologic Surgery. “About 70 percent of patients newly diagnosed with prostate cancer are in the early stages, meaning the cancer is confined to the prostate gland, and they have nonaggressive tumors. As such, these patients have an excellent prognosis without surgery. This study confirms that aggressive treatment usually is not necessary. We hope the findings will steer doctors away from recommending surgery or radiation to their patients with nonaggressive early-stage prostate cancer and patients away from thinking it’s necessary.”
The American Cancer Society ranks prostate cancer as the second most common cancer in men and the third-leading cause of cancer deaths among men, after lung and colorectal cancer. In 2017, about 161,360 men will be diagnosed with prostate cancer, and 26,730 will die from it.
The study, known as the Prostate Cancer Intervention Versus Observation Trial, or PIVOT, is one of the largest and longest involving cancer patients. It got underway in 1994 just as the prostate-specific antigen blood test for prostate cancer became routine. With many more men diagnosed with prostate cancer, the standard treatment for all prostate cancers became surgery or radiation, with the thinking that removing or irradiating the tumor would increase survival. But over the next decade, reports of treatment-related complications raised concerns, as did data indicating that most early-stage cancers grew so slowly they were unlikely to cause health problems.
To evaluate any potential benefits of surgery, the researchers randomly assigned 731 men in the U.S. with localized prostate cancer to receive either surgery or observation at one of 44 Department of Veteran Affairs Health Care Centers or eight academic medical centers, including Washington University. The average age of men in the study was 67 at the time of enrollment.
Of the men who had prostate cancer surgery, 223 (61 percent) died of other causes after up to 20 years of follow-up, compared with 245 men (66 percent) in the observation group – a difference that is not statistically different. Further, 27 (7 percent) men in the surgery group died of prostate cancer, compared with 42 men (11 percent) in the observation group, but that difference also is not statistically significant.
However, the data show that surgery may have a mortality benefit in some men, particularly those with a long life expectancy and intermediate-risk prostate cancer. (Such men generally have PSA scores of 10-20 ng/ml and a Gleason score of seven. The latter score signifies tumor aggressiveness.)
“It would be a disservice to dismiss surgery as a viable option for patients with intermediate-risk prostate cancer,” said Andriole, the School of Medicine’s Robert K. Royce Distinguished Professor of Urologic Surgery. He treats patients at Siteman Cancer Center at Barnes-Jewish Hospital and Washington University. “For these patients, and for some men with high-risk prostate cancer, surgery is often beneficial, as are other treatments such as radiation.”
Technology has advanced since the study began, allowing physicians to more accurately classify tumors and avoid overtreating patients who have prostate cancer.
Of the 364 men treated with surgery, 53 (15 percent) suffered from erectile dysfunction, and 63 (17 percent) reported having incontinence. Another 45 developed other complications.
“The benefits of surgery also need to be balanced against the negative long-term consequences of surgery that occur early and often,” said senior author Timothy Wilt, MD, a physician-researcher with the Center for Chronic Disease Outcomes Research at the Minneapolis VA Health Care System and a professor of medicine at the University of Minnesota. “Our results demonstrate that for the majority of men with localized prostate cancer, selecting observation for their treatment choice can help them live a similar length of life, avoid death from prostate cancer and prevent harms from surgical treatment. Physicians can use information from our study to confidently recommend observation as the preferred treatment option for men with early prostate cancer.”







