Startup company founded by Washington University scientists acquired by Eli Lilly
Drugmaker purchases Disarm Therapeutics to develop treatments for neurodegenerative diseases
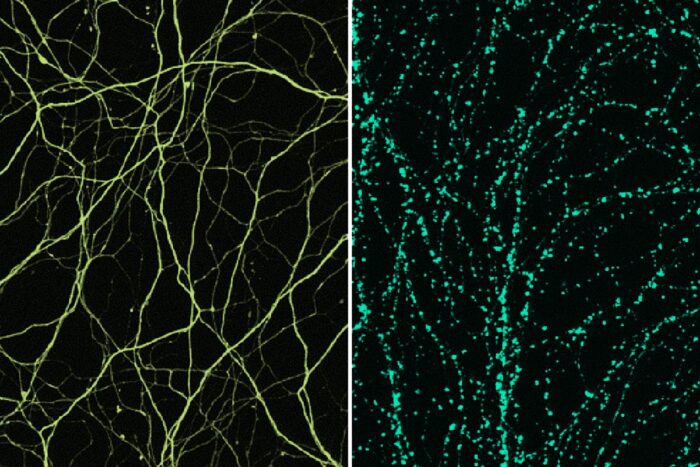 Josiah Gerdts/Milbrandt lab
Josiah Gerdts/Milbrandt labNerve axons (left) serve as the electrical wiring of the nervous system. According to Washington University research, a molecule called SARM1 triggers a self-destruct program in axons that leads to their degeneration (right), a process common to many neurodegenerative diseases. Researchers at Washington University School of Medicine in St. Louis founded a startup company, Disarm Therapeutics, to develop drugs that block this process. Pharmaceutical company Eli Lilly purchased Disarm to boost the drug development process. Both images show mouse axons with yellow and green added for clarity.
Pharmaceutical maker Eli Lilly and Company has purchased Disarm Therapeutics, a startup biotechnology firm founded by researchers at Washington University School of Medicine in St. Louis. Disarm Therapeutics was co-founded by Jeffrey Milbrandt, MD, PhD, and Aaron DiAntonio, MD, PhD, to speed the development of treatments for multiple neurodegenerative conditions.
Based on research from the Milbrandt and DiAntonio labs, the researchers’ startup company was developing drugs aimed at blocking or slowing axonal degeneration, a common problem across numerous neurological disorders. Such drugs potentially could help millions of patients with debilitating nerve damage due to a variety of ailments and injuries.

“Disarm Therapeutics had reached the point in the drug development process where we either needed to raise much more funding ourselves or work with a pharmaceutical company with the infrastructure already in place to take this technology to the next level,” said Milbrandt, the James S. McDonnell Professor, head of the Department of Genetics, and executive director of the McDonnell Genome Institute at the School of Medicine.
Lilly made the acquisition, announced Thursday, Oct. 15, with an upfront payment of $135 million. If future development, regulatory and commercial milestones are met, Disarm investors may be eligible for up to $1.2 billion in additional payments.
“This is a wonderful reflection of outstanding research being done by Jeff Milbrandt and Aaron DiAntonio,” said David H. Perlmutter, MD, executive vice chancellor for medical affairs, the George and Carol Bauer Dean of the School of Medicine, and the Spencer T. and Ann W. Olin Distinguished Professor. “Washington University researchers are carrying out deeply important cutting-edge research, and the more we can help our investigators connect the dots between their basic and translational research and industry partners, the more we will be able to realize our unique potential for improving the health of our patients through novel therapies.”
He added: “The Office of Technology Management (OTM) and the entrepreneurial support available to our researchers have been key to the success of Disarm, and we are enormously proud that this exciting research program at Washington University has reached the next milestone in the journey to FDA-approved drugs that help patients with devastating neurological disorders.”
The causes of neurological disorders are numerous and diverse, but one common element among such disorders is the loss of axons — the nervous system’s wiring, responsible for zapping electrical signals from one nerve cell to another. Such axonal loss can be devastating and can lead to a wide range of disorders, from peripheral neuropathy, traumatic brain injury and glaucoma, to multiple sclerosis, amyotrophic lateral sclerosis (ALS) and Parkinson’s disease.

In recent years, Milbrandt, DiAntonio — the Alan A. and Edith L. Wolff Professor of Developmental Biology — and their colleagues have demonstrated that injured or diseased axons initiate a self-destruction program. Blocking this program provides a way to stop axonal loss, a discovery that has shown promise as a treatment for a wide variety of neurodegenerative diseases.
In 2017, scientists led by Milbrandt and DiAntonio showed that a molecule called SARM1 is the main culprit in the loss of axons in peripheral nerves following damage from a common chemotherapy drug called vincristine.
The researchers further showed that SARM1 is an enzyme — a molecule that carries out biochemical reactions. This was surprising because SARM1 belongs to a class of molecules that had, up to that point, been shown to serve as cellular scaffolds that provide support for other proteins to carry out their activities.
“No one had ever shown that this type of molecule could be an enzyme,” DiAntonio said. “So we went into our experiments assuming SARM1 was only a scaffold and that there must be some other enzyme responsible for demolition of the axon. We essentially searched for a demolition crew, only to discover that the scaffold itself is destroying the axon. It’s the last thing you would expect.”
In this case, SARM1 was destroying axons by burning through all the cellular fuel that axons need to function and stay alive. They found that this enzyme is the “central executioner” of damaged axons across many organisms — including mice, rats, flies, fish and, importantly, in human neurons. Activated SARM1 triggers axons to self-destruct, kicking off a chain of events that quickly consumes all of a nerve cell’s energy supply. The axons of such cells break into pieces. If drugs could be found that blocked SARM1, then these could serve as a therapy that protects axons from destruction.
“SARM1 triggers a loss of axons that happens in almost all neurodegenerative diseases,” DiAntonio said. “Blocking SARM1 is not going to cure these diseases — there’s something else wrong that is leading to SARM1 being activated — but if you can keep the neurons connected, the hope is that that would have a significant impact for people with a wide array of neurological diseases or injuries.”
To help translate their discoveries into potential therapies that could help patients, Milbrandt and DiAntonio received funding from Washington University’s Leadership and Entrepreneurship Acceleration Program (LEAP). Additional support came from BioSTL’s BioGenerator program. The researchers then collaborated with Confluence Therapeutics in the Cortex Innovation Community to strengthen the commercialization prospects of their technology.
Working with Washington University’s Office of Technology Management, Milbrandt and DiAntonio founded Disarm Therapeutics to help develop technologies based on their discoveries involving SARM1 and the potential benefits of blocking it to protect nerves from destruction. The investors in Disarm Therapeutics were Atlas Venture Capital along with Lightstone Ventures and Abbvie Ventures.
“Washington University’s Office of Technology Management played an important role in helping us get Disarm Therapeutics started,” Milbrandt said. “The guidance they provided, along with the expertise of the collegial and growing network of St Louis-based biopharmaceutical entrepreneurs, were essential to the successful creation of this new company.”
Added Nichole R. Mercier, PhD, assistant vice chancellor and managing director of the Office of Technology Management: “We were happy to partner with Dr. Milbrandt and Dr. DiAntonio to help facilitate the launch of Disarm Therapeutics as a Washington University startup. We’re excited to see the success of the technology and contribute to fulfilling the mission of OTM — pairing this type of cutting-edge research with the business expertise of our office to have a positive impact on society.”
The small molecule SARM1 inhibitors developed at Disarm Therapeutics hold promise for patients with neurodegenerative conditions including peripheral neuropathy resulting from chemotherapy or neuropathy due to complications of diabetes, Milbrandt said. Peripheral neuropathy affects about 20 million people in the United States.
“It would be very fulfilling to see our work investigating a fundamental problem in neuroscience become a treatment to help patients with these disorders,” Milbrandt said. “Our experience in starting a company is a wonderful example of how the environment at Washington University facilitates partnerships between scientists and industry, with the goal of turning basic science discoveries into therapeutic advances.”
Added DiAntonio: “What’s always been exciting about SARM1 is that it’s not related to a single disease; it’s related to a disease process that occurs in almost every neurodegenerative disease. The potential for SARM1 is huge. Having a major pharmaceutical company pushing it forward will increase the chances that these therapies we started will actually make a difference in helping patients.”







