School of Medicine joins exclusive pediatric neuro-oncology consortium
Expands treatment options for children with brain tumors
 E. Holland Durando
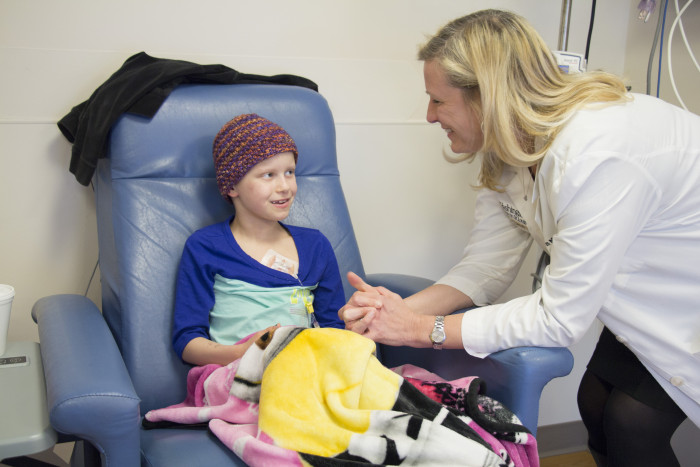
E. Holland DurandoThe School of Medicine's Karen Gauvain, MD, visits with Madeline Thompson, 8, at St. Louis Children's Hospital, where the young patient has been receiving treatment for a brain tumor.
In less than a year, Madeline Thompson, 8, learned she had a brain tumor, underwent two surgeries and endured extensive chemotherapy.
“There was a point when it didn’t look good for Maddie, and I had to prepare for the worst,” said her mother, Katra Thompson. “But today she is as close to cancer-free as possible.”
Thompson, of Hannibal, Mo., credited the Pediatric Neuro-Oncology staff at Washington University School of Medicine in St. Louis and St. Louis Children’s Hospital.
“Everyone is so devoted to making Maddie better,” said Thompson, who shared popcorn with her daughter on a recent afternoon while Maddie received treatment. “I am so happy Maddie can go here because the doctors and staff are the best in the industry.”
Others agree. The Pediatric Neuro-Oncology program recently joined a prestigious network of the nation’s top childhood cancer centers. That development widens treatment options for children whose brain tumors don’t respond to standard care.
The network, the Pacific Pediatric Neuro-Oncology Consortium, provides physicians with access to the latest technologies as well as clinical trials at its 15 medical centers, thereby expanding overall treatment options, and, ideally, patient success rates, said the program’s co-directors: the School of Medicine’s Joshua B. Rubin, MD, PhD, professor of pediatrics and of neuroscience; and David D. Limbrick, MD, PhD, an associate professor of neurological surgery and of pediatrics.
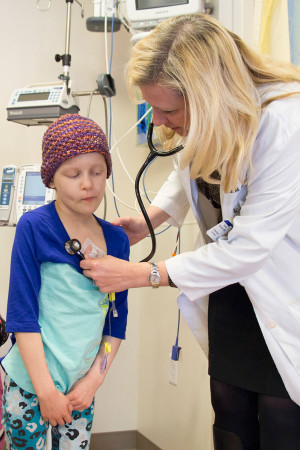 E. Holland Durando
E. Holland DurandoPhysicians and staff within the consortium can share data, expertise and resources regarding brain tumor biology and possible new treatments, said Rubin, who is also co-leader of the Solid Tumor Therapeutics Program for Washington University’s Siteman Cancer Center. “Being a part of the consortium brings cutting-edge brain tumor therapies to the children of St. Louis and the surrounding region.”
Added Limbrick: “As part of the consortium, we are better able to offer our patients the option of participating in clinical trials for personalized treatments for their brain tumors and to be part of the larger movement to understand the molecular basis of brain tumors.”
The School of Medicine’s program offers individualized treatment plans through a multi-disciplinary approach that involves pediatric neuro-oncologists, neurosurgeons, radiation oncologists, radiologists, pathologists, endocrinologists, psychologists, social work, nurses and other specialty staff. The team meets weekly to evaluate every child’s unique needs.
“The treatment of pediatric brain tumors is complex,” said Karen Gauvain, MD, an assistant professor of pediatrics in the Division of Pediatric Hematology/Oncology. “A child needs skilled, compassionate care from many medical specialties.
“Our care also is long-term,” added Gauvain, who oversees and manages clinical trials as Washington University’s principal investigator for the consortium. “We are with a child from initial diagnosis to after-care rehabilitation, such as speech, occupational and physical therapy, to follow-up in both the home and school.”
The neuro-oncology program provides top-of-the-line imaging technology and neurosurgical approaches. Children’s Hospital is one of the few pediatric medical centers that offers intraoperative MRI, considered a major advance in the treatment of brain tumors because it allows neurosurgeons to remove tumors more precisely, thanks to MRI images and computer guidance during surgery. The Pediatric Neuro-Oncology program is also the first to ever evaluate laser ablation surgery for pediatric brain tumors in a clinical trial.
Pediatric brain tumor patients also benefit from state-of-the-art radiation therapy, including intensity-modulated radiation therapy (IMRT), proton beam radiation and radiosurgery. “We are so fortunate to be able to provide all of these radiation services for our pediatric brain tumor patients,” said Stephanie Perkins, MD, assistant professor of radiation oncology and chief of the pediatric radiation oncology service.
Research in the Pediatric Neuro-Oncology Program is supported by the pediatric brain tumor bank, which houses 5,300 tumor, 800 blood and a growing number of cerebrospinal fluid specimens. Each specimen is meticulously annotated with clinical data and available to scientists worldwide whose research is aimed at life-saving treatments for children with brain tumors. Past and ongoing clinical studies utilizing these specimens have contributed to, among other things, the definition of molecular subtypes of medulloblastoma, the most common childhood malignant brain tumor.
Patients and their families must provide consent before surgeons can collect tissue specimens. “Most families embrace it,” Rubin said. “Their children are helping to advance science. They see it as a way to turn something bad into something good.”
The tumor bank and The McDonnell Genome Institute, one of three large-scale genome sequencing centers funded by the National Institutes of Health (NIH), are working together to develop new insight and approaches for personalizing tumor treatments. The ultimate goal, researchers said, is to tailor an approach to interrupting the mutations and cellular pathways that drive each child’s unique cancer.
 Robert Boston
Robert Boston






