Rapid Ebola diagnosis may be possible with new technology
Faster diagnosis could help limit deadly outbreaks
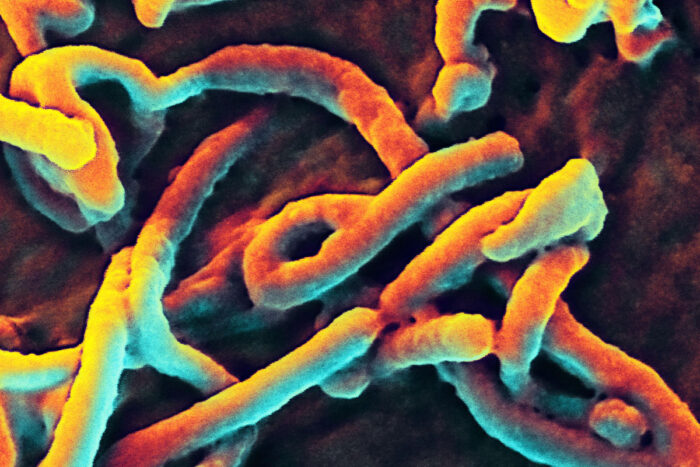 National Institute of Allergy and Infectious Diseases
National Institute of Allergy and Infectious DiseasesPictured is a colorized scanning electron microscopic image that depicts Ebola virus particles budding from the surface of a cell. A new study from researchers at Washington University School of Medicine in St. Louis and colleagues at other institutions details a new tool that can quickly identify the presence of Ebola virus in blood samples. The technology has potential to be developed into a rapid diagnostic test.
A new tool can quickly and reliably identify the presence of Ebola virus in blood samples, according to a study by researchers at Washington University School of Medicine in St. Louis and colleagues at other institutions.
The technology, which uses so-called optical microring resonators, potentially could be developed into a rapid diagnostic test for the deadly Ebola virus disease, which kills up to 89% of infected people. Since it was discovered in 1976, Ebola virus has caused dozens of outbreaks, mostly in central and west Africa. Most notable was an outbreak that began in 2014 and killed more than 11,000 people in Guinea, Sierra Leone and Liberia; in the U.S., the virus caused 11 cases and two deaths. A rapid, early diagnostic could help public health workers track the virus’ spread and implement strategies to limit outbreaks.
The study — which also involved researchers from the University of Michigan, Ann Arbor, and Integrated Biotherapeutics, a biotech company — is published June 8 in Cell Reports Methods.
“Any time you can diagnose an infection earlier, you can allocate health-care resources more efficiently and promote better outcomes for the individual and the community,” said co-first author Abraham Qavi, MD, PhD, a postdoctoral researcher at Washington University. “Using a biomarker of Ebola infection, we’ve shown that we can detect Ebola infection in the crucial early days after infection. A few days makes a big difference in terms of getting people the medical care they need and breaking the cycle of transmission.”
Ebola virus is transmitted by contact with bodily fluids. It causes fever, body aches, diarrhea and bleeding — nonspecific symptoms that easily can be mistaken for other viral infections or for malaria. In recent years, vaccines and effective therapies for Ebola have been developed, but they are not widely available. Instead, health officials control the deadly virus by containing outbreaks. The strategy relies on quickly identifying infected people and preventing transmission by encouraging caregivers to wear protective gear.
Qavi had previously worked with Ryan C. Bailey, PhD, the Robert A. Gregg Professor of Chemistry at the University of Michigan and a co-senior author on this paper, to co-develop optical microring resonators, a kind of whispering gallery mode device used for molecular detection. The name comes from the Whispering Gallery at St. Paul’s Cathedral in London. A whisper uttered on a walkway in the dome above the nave can be heard clearly more than 100 feet away because the sound waves increase in amplitude as they bounce around the circular wall. The 18th century builders accidentally constructed a giant demonstration of the principle of acoustic resonance, in which sound waves increase in amplitude if they interact in precisely the right way. The same phenomenon occurs with light waves on a much smaller scale.
When Qavi joined the lab of co-senior author Gaya K. Amarasinghe, PhD — an Ebola expert and the Alumni Endowed Professor of Pathology & Immunology and a professor of biochemistry & molecular biophysics and of molecular microbiology at Washington University — they decided to apply the technology to create a better diagnostic test for Ebola. Qavi teamed up with Bailey, co-first author Krista Meserve, a graduate student in Bailey’s lab, and co-author Lan Yang, PhD, the Edwin H. and Florence G. Skinner Professor of Electrical & Systems Engineering at Washington University’s McKelvey School of Engineering, to develop a tool that could detect tiny amounts of Ebola-related molecules in blood samples using microring resonators.
“We trap light in the resonators and use resonance to enhance and boost our signal,” Qavi said. “By monitoring where this resonance wavelength occurs, we can tell how much of the molecule we have.”
The key was finding the right molecule. Current diagnostic tests detect the virus’s genetic material or a glycoprotein — a protein covered in sugar — produced by the virus. But they aren’t reliable until the virus has multiplied to high levels in the body, a process that can take days. Co-senior author Frederick Holtsberg, PhD, vice president of manufacturing and bioanalytics at Integrated Biotherapeutics, developed a highly sensitive antibody capable of detecting the viral soluble glycoprotein at low levels.
The researchers incorporated the antibody into their device and tested it using blood from infected animals. They found their technique could detect the glycoprotein as early as or earlier than the most sensitive test for viral genetic material. Importantly, the technology also allowed them to quantify the amount of viral glycoprotein in the blood. The higher the level, the worse the infected animals fared. Moreover, the test only took 40 minutes start to finish.
“Looking at these data, we can say, ‘If you’re above these levels, your chance of survival is low; if you’re below it, your chance of survival is high’,” Qavi said. “We still have to validate this in infected individuals, but if it holds up, doctors could use this information to tailor treatment plans for individual patients and allocate scarce medications to the patients most likely to benefit.
“We’ve shown the fundamental science works,” he added. “Now it’s just an issue of miniaturizing the devices and taking them into the field.”







