Racial differences in Alzheimer’s research focus of $15 million grant
Study investigates whether biological markers of Alzheimer’s in white patients also apply to African Americans
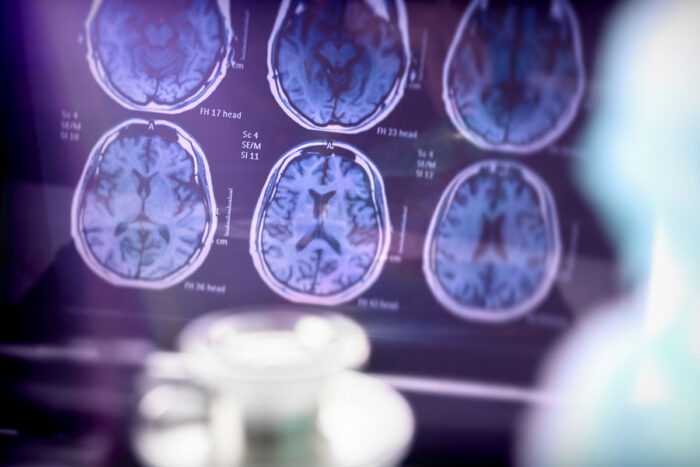 Getty Images
Getty ImagesPictured are brain scans, which can be used to image plaque and protein tangles characteristic of Alzheimer's disease. A new grant for research at Washington University School of Medicine in St. Louis focuses on brain scans and other markers of Alzheimer's. Early markers of disease mainly have been identified in white populations. The study's goal is to establish whether these disease markers also apply to African Americans, who are underrepresented in Alzheimer's research.
In efforts to identify who is at risk of developing Alzheimer’s dementia, researchers over the years have zeroed in on several signs — or biological markers — that indicate early stages of the disease. If individuals could be identified long before symptoms of dementia begin to appear, doctors could target those patients with future preventive therapies.
But those early markers of disease — whether found in blood, cerebrospinal fluid or brain scans — have been identified primarily in white populations. Whether these disease markers also apply to African Americans remains an open question.
A $14.6 million grant to Washington University School of Medicine in St. Louis will support studies to investigate whether early markers of Alzheimer’s that have shown promise for predicting the disease in white populations also predict the disease in African Americans. The researchers also will seek biological and social determinants of health that may explain the possible racial differences in these markers.
“Past studies have produced conflicting data about African Americans and Alzheimer’s disease,” said Chengjie Xiong, PhD, a professor of biostatistics and interim director of the Division of Biostatistics within the Institute for Informatics. “Mainly, the problem is that the sample sizes of African Americans in any given study are too small to be able to draw definitive conclusions about the disease in African American populations. We want to understand whether Alzheimer’s is, in fact, the same disease in white and African American populations, both in the silent stage before symptoms and in the symptomatic stage.”
The researchers will combine existing data from earlier studies to obtain a larger sample size of African Americans. They also will add prospectively collected data from new studies currently underway; these include investigations of Alzheimer’s disease markers in this underrepresented population and how the markers change over time. The researchers will re-analyze existing samples and brain scans collected from past participants along with prospectively collected samples and scans, including cerebrospinal fluid, MRI scans and positron emission tomography (PET) scans. The cerebrospinal fluid samples and imaging scans can reveal the presence of protein plaques and tangles in the brain — called amyloid plaques and tau tangles — that build up silently for a long period of time and eventually interfere with cognition.
The ongoing clinical and biomarker studies that will be incorporated into this analysis include studies being conducted at the Washington University Knight Alzheimer Disease Research Center, the University of Pennsylvania Alzheimer Disease Core Center, the Emory University Alzheimer Disease Research Center, the Harvard Aging Brain Study, and the Anti-Amyloid Treatment of Asymptomatic Alzheimer’s trial.
The harmonization of clinical and cognitive data across the studies will be led by John Morris, MD, the Harvey A. & Dorismae Hacker Friedman Distinguished Professor of Neurology and director of the Knight Alzheimer Disease Research Center; and Jason Hassenstab, PhD, an associate professor of neurology and the psychometrics leader of the center. The central reprocessing of the samples and scans across the studies will be led by Anne Fagan, PhD, a professor of neurology; and Tammie Benzinger, MD, PhD, a professor of radiology, who lead the Fluid Biomarker Core and Neuroimaging Core of the Knight Alzheimer Disease Research Center. The recruitment will be led by Joyce Balls-Berry, PhD, an associate professor of neurology and the leader of the Health Disparities and Equity Core.
Altogether, the effort will include a total of over 1,000 African American participants and will produce adequate statistical power required to assess biologically significant differences that might exist between the markers of Alzheimer’s disease in white participants and those in African American populations. For example, one question the researchers would like to answer is whether the protein tau is as important in African American populations as it seems to be in white populations.
“There is some evidence, though it’s not conclusive, that middle-aged and elderly African Americans have lower levels of tau in the cerebrospinal fluid than white people of similar ages,” Xiong said. “If this is true and a treatment is developed that reduces tau levels, it’s possible it won’t work well in African Americans. Understanding the disease in African Americans is crucial and will help guide the development of effective treatments.”







