Podcast: Vaccines have arrived but COVID-19 treatments progressing much more slowly
This episode of 'Show Me the Science' contrasts the rapid development of effective vaccines with the lack of progress toward effective therapies
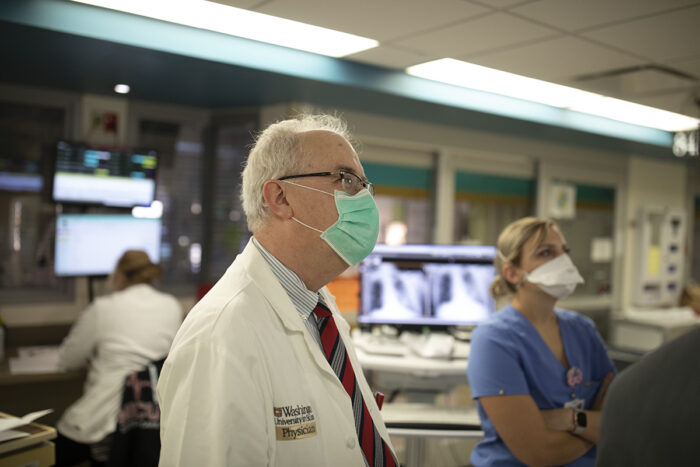 Matt Miller
Matt MillerWilliam G. Powderly, MD, discusses COVID-19 cases with staff in the intensive care unit at Barnes-Jewish Hospital. Powderly says that although vaccine development has been rapid, the search for therapies for patients infected with the novel coronavirus has been less successful.
A new episode of our podcast, “Show Me the Science,” has been posted. At present, these podcast episodes are highlighting research and patient care on the Washington University Medical Campus as our scientists and clinicians confront the COVID-19 pandemic.
COVID-19 vaccine development has been rapid and successful. Two vaccines that report more than 90% efficacy against the virus already are in use, with approval of more vaccines expected in the coming weeks. Meanwhile, the development of treatments for those infected with the virus has been slower. Only one drug, the steroid dexamethasone, has been proven to reduce the risk of death in those hospitalized with COVID-19. In this episode, we’ll hear reasons why the development of effective treatments has progressed so slowly. Discussing this with us is William G. Powderly, MD, the Larry J. Shapiro Director of the Institute for Public Health, co-director of the Division of Infectious Diseases at Washington University School of Medicine in St. Louis and director of the university’s Institute of Clinical and Translational Sciences. He says one reason development of therapies has been slow is because there haven’t been enough big, well-controlled studies. We’ll also hear from Eric J. Lenze, MD, the Wallace and Lucille Renard Professor of Psychiatry, and Angela M. Reiersen, MD, an associate professor of psychiatry. They led a preliminary study at the School of Medicine in which a psychiatric drug was used to keep people with COVID-19 from getting sick enough to be hospitalized. Their study was successful. Now they’re expanding the trial to include COVID-19 patients in all of the United States.
The podcast, “Show Me the Science,” is produced by the Office of Medical Public Affairs at Washington University School of Medicine in St. Louis.
Transcript
[music]
Jim Dryden (host): Hello, and welcome to Show Me the Science, conversations about science and health with the people of Washington University School of Medicine in St. Louis, Missouri, the Show-Me State. As we continue to detail Washington University’s response to the COVID-19 pandemic, we focus in this episode on treatments. We know that vaccines already are being given, but thousands more will get infected between now and the time the vaccines are more widely available.
William Powderly, MD: As we reflect on things that went well and things that did not go well with this epidemic, one of them, I think, has to be how poorly we did as a country in coordinating our clinical research into this disease for treatment. We’ve done a wonderful job for a vaccine. I think we’ve done a very poor job for therapeutics.
Dryden: That’s Dr. William Powderly, co-director of the Division of Infectious Diseases at Washington University. He says that, although vaccines give us reason to hope, current infection rates mean we’re facing a few months of sick people who could benefit from effective treatments, treatments that, at least so far, don’t really exist. A possible exception is the psychiatric drug, fluvoxamine. Washington University psychiatrist Eric Lenze and his colleagues began testing that drug in COVID-19 patients last spring. The initial study in the St. Louis region was very successful. The drug was shipped to people’s homes, and no one who took fluvoxamine went on to develop severe disease. Now Lenze’s team is trying to replicate those findings in COVID-19 patients from all 50 states.
Eric Lenze, MD: For the next study, it won’t matter whether you live 2 miles away from us in St. Louis, or 1,000 miles away from us in rural New Mexico. If you have COVID and recently tested positive, you’d be eligible for the study, and we’d bring the trial to you.
Dryden: We’ll get to the story of why a bunch of psychiatrists thought that a drug used mainly to treat obsessive-compulsive disorder might also keep COVID-19 at bay. But first, back to the bigger treatment picture. Powderly says that, where vaccine development has been rapid, finding effective treatments has been much slower.
Powderly: Unlike vaccines, we haven’t really yet made a breakthrough in terms of treatment. But if I can step back for a moment, what I will say, first of all, is that, overall, it appears that the case fatality rate, that is, the likelihood of dying, seems to have come down since the very beginning of the epidemic. I think that reflects not so much advances in treatment, although there have been some, but really advances in overall care and the recognition in our hospitals of the sort of things that improve care and survival in general. For example, early in the epidemic, we recognized that blood clots were a significant contributor to morbidity and, potentially, mortality. So there’s been a much more deliberate approach to using blood thinners and anticoagulation in patients. Our pulmonary and critical-care specialists have become much more adept at managing ventilation. Initially, I think they were ventilating a lot of people very quickly. But then people recognized this disease behaves differently, and it needed a different approach. So when you think about treatment, what you need is a sort of biphasic approach. At the very beginning, you need drugs that will interfere with the virus. But when you get into the hospital stage, you need drugs that would potentially interfere with the immune system. And by far, the most successful drug we have in bringing down the mortality of this disease is, in fact, dexamethasone, which is a steroid, which is sort of a cannonball blast to the immune system to try to dampen it down. And that is, so far, the only drug that has been shown to have a benefit on mortality, that is, to decrease the likelihood of dying.
Dryden: You’re currently heading up, though, a trial of some other drugs that may be helpful in those same patients, correct?
Powderly: I am currently chairing an NIH study that is actively enrolling patients with moderate-to-severe COVID who are in hospital, to try and look at three different agents. We’re in this situation where, with the exception of dexamethasone, we don’t have anything that has had a dramatic effect on survival. The steroids work, but by dampening down the immune system so much you run the risk that patients will get other problems related to their immune system being dampened. And we worry about other infections in that circumstance in particular. At the early phase, there has been a tremendous amount of interest in monoclonal antibodies. The theory there is that you could give patients, if you identify them early, drugs that interfere with the virus itself. And the first group of drugs that were really investigated were a series of monoclonal antibodies. And they’ve had a modest effect. If you give them to people who have symptoms in the early phase, you can reduce their risk of being hospitalized. One of the ways we approach this is, how many people do you need to treat to benefit one person? For these drugs, you need to treat 20 to 25 people to benefit one person. If you were target it to just high-risk patients, older people, you might be able to treat eight to 10 to benefit one. We had hoped that, if we were to give those drugs to patients when they came into hospital with more severe illness, that might be beneficial. But unfortunately, in those trials, there was no benefit.
Dryden: Now, before we called this “SARS-CoV-2,” at least in the media, we called it “the novel coronavirus.” A novel virus had not been seen before. Is that the basic explanation for why some of these repurposed drugs haven’t been working as well? Because this is a novel virus that we don’t completely understand yet?
Powderly: I think that’s absolutely true, Jim. It’s part of the issue. As you said, it was a new virus, and we made inferences from other viruses. We made inferences from viruses, like influenza, that in general would cause a mild illness, but occasionally can cause a severe illness that has a respiratory component, and people could end up in the ICU. Those sort of inferences were reasonable, but it turned out that, actually, what’s going on with this virus is probably quite different. And in fact, one of our young faculty, Phil Mudd, had been studying influenza. And what he has shown is that the immune responses that are triggered, and the whole pathway that, actually, is activated is very different. It was not inappropriate to try these drugs. And in fact, one of the drugs that was looked at, remdesivir, has shown a modest benefit, but again, had no effect on survival. This disease is so variable and unpredictable that you actually need to have placebo-controlled trials. So there were a lot of studies that were done. And the classic example was in the early days— were these uncontrolled studies of drugs, like hydroxychloroquine, which led to a lot of people thinking that drugs might be beneficial. But because they had no control group, it turned out that the benefit that was seen was random. When you’re dealing with a mild disease, where 80% or 90% of the people, depending on who you’re studying, are going to get better anyways, it becomes essential to do randomized controlled trials. And you have to do pretty large randomized controlled trials. You have to have hundreds of patients, if not thousands of patients, in your study. One of the really novel approaches to how to do this has actually been led here by Eric Lenze with an approach that is completely remote.
Dryden: That study is just beginning to recruit nationally now. I mean, their pilot study had some fairly good results. But again, you don’t know how many of those people would have not progressed, whether they were on the drug or not.
Powderly: Yeah. I will say this, that Eric Lenze and his colleagues did the right thing from the beginning. They did a placebo-controlled trial. It was small, and it was a proof-of-concept. And it did show a benefit for the drug that they were repurposing, fluvoxamine. What it now requires is a larger, multicenter study, which they’re just starting. As we reflect on things that went well and things that did not go well with this epidemic, one of them, I think, has to be how poorly we did as a country in coordinating our clinical research into this disease for treatment. We’ve done a wonderful job for a vaccine. I think we’ve done a very poor job for therapeutics.
Dryden: We’ll get back to that point and talk about some reasons in a moment, but first back to that study from Eric Lenze and his colleagues. They monitored COVID-19 patients who were isolating in their homes in the St. Louis region, testing the psychiatric drug, fluvoxamine, which is from a class of antidepressant drugs called selective serotonin reuptake inhibitors and often is used specifically in people with obsessive-compulsive disorder. None of the COVID-19 patients who took fluvoxamine got sick enough to be hospitalized. Meanwhile, six of the 72 patients who took the placebo experienced progression of their disease, and four eventually did have to go to the hospital. But none of the patients had to come to the medical center to participate in the study. Instead, the researchers shipped the drug or an inactive placebo, as well as thermometers and other medical equipment, to the homes of people in the study. And they monitored them online and over the phone.
Lenze: Yeah, traditionally, clinical trials are done requiring a lot of patients having to come into the medical center for visits. We’ve been moving more towards a more patient-centered model, which we call “fully remote trials.” Basically, you take the trial to the patient rather than the patient to the trial. And that’s what we did in this study, partly because we had to. This study was done at the early height of the pandemic. We were on a lockdown. And of course, patients had COVID. They had a highly contagious, dangerous disease and needed to be self-isolated.
Dryden: Does the fact that you were able to do this remotely make it easier to expand it to a bigger— you know, as great as the finding is that nobody who took the drug ended up going to the hospital, you’d like to have that be replicated in a larger number of patients, right?
Lenze: Yeah, that’s right. We think it’s critical to confirm these findings in a larger study. The essence of science is replication, right? And so the one study is a great preliminary finding, but we need to confirm it. So for the next study, it won’t matter whether you live 2 miles away from us in St. Louis, or 1,000 miles away from us in rural New Mexico. If you have COVID and recently tested positive, you’d be eligible for the study, and we’d bring the trial to you.
Dryden: One reason they chose to study fluvoxamine was because of something that one of Lenze’s colleagues had observed when examining young patients who have a very rare diabetes-like disease known as Wolfram syndrome.
Angela Reiersen, MD: I’m Angela Reiersen. I’m an associate professor of psychiatry. I’m a child and adolescent psychiatrist.
Dryden: Reiersen had been doing psychiatric evaluations of children and teens with Wolfram syndrome. People with Wolfram syndrome have all sorts of problems, including diabetes and neurological issues. And Reiersen found that some of the issues patients were having with drugs used to treat depression and anxiety may have been linked to a part of their body’s immune systems that also has been connected to some of the serious deterioration experienced by people infected with the SARS-CoV-2 virus.
Reiersen: I’ve been working with the Wolfram Syndrome Research Clinic for the past few years. And one of my observations was that people with this syndrome were reporting reduced responses to certain medications. And in doing some research, I found that antidepressants have varying activity at something called a sigma-1 receptor. And it seemed that the responses to the medication had to do with the action at that particular receptor. A sigma-1 receptor has some anti-inflammatory effects, where in the response to inflammatory triggers, drugs that activate this receptor can reduce the production of cytokines.
Dryden: And cytokines are molecules that are involved in the inflammatory response that the body mounts to an infection or something like that?
Reiersen: Right. And so then in March 2020, when I heard that, in some cases of COVID-19, people have worsening of their symptoms around week two due to an excessive inflammatory response, I thought, “Well, maybe we could use a sigma-1 agonist, fluvoxamine, to try and treat this and prevent the clinical deterioration.”
Lenze: How about the fact that a bunch of psychiatrists came up with a treatment for COVID? Talk about adding 2 and 2 together and getting 11. The idea that Angela was able to combine a review of the literature on COVID, with an article that came out last year on fluvoxamine for sepsis, and her own clinical experiences with Wolfram syndrome, and you combine all that together into this hypothesis, is just— I don’t know. If this finding is actually confirmed, then that’s going to just go down, I think, in the annals of just, like, one of the most amazing conjectures, up there with the guy who came up with the idea that “Maybe bacteria cause peptic ulcer disease.” And everyone thought he was an idiot for proposing such a ridiculous idea, which, of course, now it’s been proven, and it’s changed treatment, so…
Reiersen: It supports also just the importance of studying rare diseases, because sometimes people think, “Why should we spend money on rare diseases? There’s not that many people that have them. It may not help that many people.” But by studying rare diseases and looking at the mechanisms involved, you never know when that’s going to apply to some other field that seems completely unrelated.
Lenze: Based on what we proposed to be the mechanism of fluvoxamine, it seems that it would be most useful in people who have just gotten COVID, just started to get symptoms, but haven’t yet gotten extremely ill.
Dryden: Lenze and Reiersen and their colleagues now are testing that in patients from throughout the United States, hoping to recruit 1,100 people who’ve recently been infected. And if fluvoxamine turns out to work in those patients, then Powderly, the infectious diseases specialist, says it could help a lot as people continue to get infected even as the hope of a vaccine lurks on the horizon.
Powderly: The NIH and federal government’s response to vaccines, Operation Warp Speed, I think, was remarkable. Really having a strategy that was executed in a remarkable speed. You know that there’s been some concern about the speed. But, in fact, we didn’t cut any corners. We just did things quickly in parallel and with incredible efficiency. Unfortunately, we haven’t taken the same approach to therapeutics. I don’t want to overstate it, but the science behind vaccines was the application of many, many years of vaccine technology to a new virus. The scientific pathway was more straightforward. From the perspective of therapeutics, we didn’t completely understand and still don’t completely understand how the virus, ultimately, leads to death. I think one of the things that strikes me is that, if you look at clinicaltrials.gov, which is the national repository of all the trials, there are nearly 2,000 COVID trials, and the vast majority of them will never be finished and will never give a result.
Dryden: Why?
Powderly: Well, because most of them are uncontrolled, that is, they don’t have a placebo, or they don’t have a control arm; and most of them are too small to actually be scientifically valid. And I think, to a certain extent, we have to step back and question both, why that happens, and should it be allowed to happen again? I mean, I understand why researchers all across the country try very quickly to design studies to give answers. We did, too. We designed studies to, initially— and the reason is, obviously, people were desperate. But the reality is that we would have been better off coordinating that quickly and from the beginning. And I’ll give you one really pertinent example. We have talked about convalescent plasma as a potential treatment since March. We are now 10 months into the epidemic. We’ve given hundreds of thousands of doses of convalescent plasma to people, and we still don’t know if it works. And if we had coordinated, from the very beginning, a national effort to study this properly, we’d at least know by now whether it’s effective. I would argue that we could have done this better.
Dryden: We get flu shots every year. And if we happen to get influenza anyway— I mean, there’s Tamiflu, I guess. But I think most of us probably just take something to keep our fever under control. We stay in bed for a couple of days until we start to feel better. Yeah. Same thing if we catch a bad cold. In those cases, it seems that there just really aren’t that many antivirals used. I know that COVID-19 is much more serious, but I’m wondering if it’s just the case that there just aren’t a lot of good agents for treating respiratory viruses.
Powderly: Yes. The short answer is yes. You’re absolutely right that there aren’t that many because, in general, respiratory viruses, with certain exceptions, are mild and not life-threatening. So when you have a novel virus coming along like this, there aren’t that many drugs on the shelf. I think that the antivirals that will be developed for COVID will be new drugs because they will target specifically this virus.
[music]
Dryden: With hundreds of thousands of new infections per day, as well as thousands of deaths each day, Powderly says those new drugs can’t be developed fast enough. Show Me the Science is a production of the Office of Medical Public Affairs at Washington University School of Medicine in St. Louis. The goal of this project is to keep you informed and maybe teach you some things that will give you hope. Thank you for tuning in. I’m Jim Dryden. Stay safe.







