Podcast: Global study tests chloroquine to protect health workers from COVID-19
Trial led by top academic institutions around the world, including School of Medicine
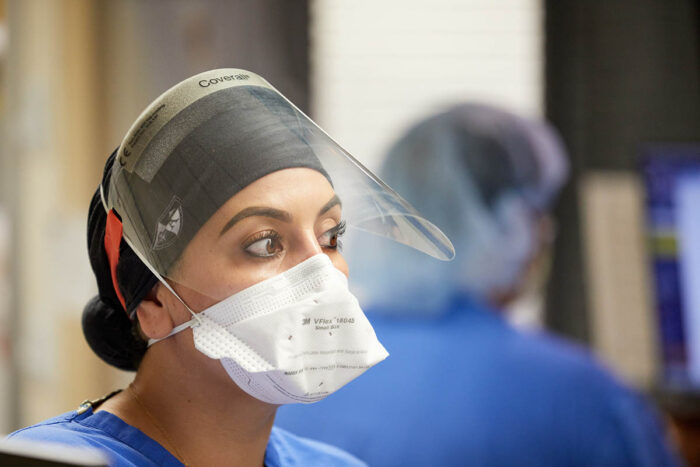 Matt Miller
Matt MillerMelissa Delavara, a registered respiratory therapist, works as a front-line caregiver with COVID-19 patients at Barnes-Jewish Hospital. Researchers at Washington University School of Medicine in St. Louis are helming a global study of an estimated 30,000 health-care workers to establish whether the antimalaria drug chloroquine might prevent or reduce the severity of COVID-19 infections in such workers.
A new episode of our podcast “Show Me the Science” has been posted. At present, these podcasts are highlighting research and patient care on the Washington University Medical Campus as our scientists and clinicians confront the COVID-19 pandemic.
More than 10% of those with serious COVID-19 infections have been front-line health-care workers. Now, an international group led by researchers at Washington University School of Medicine in St. Louis is launching a trial to see whether the drug chloroquine might help those workers. The drug trial won’t treat doctors, nurses and others after they get sick. Instead, the health-care workers will take medication prophylactically, to see whether it might be worth adding low doses of chloroquine to other personal protective equipment, such as masks, gowns and gloves.
Michael Avidan, MBBCh, the Dr. Seymour and Rose T. Brown Professor and head of the Department of Anesthesiology, is leading the study, which has sites in England, Ireland, Africa, Canada, and South America. The group is called the CROWN Collaborative (COVID Research Outcomes World Network). With funding from the COVID-19 Therapeutics Accelerator — an initiative launched by the Bill & Melinda Gates Foundation Wellcome, Mastercard and an array of public and philanthropic donors — the researchers want to learn whether low doses of chloroquine can keep health-care workers from getting COVID-19 at all or, if they do get sick, whether treatment with the drug might lead to less severe symptoms.
The podcast, “Show Me the Science,” is produced by the Office of Medical Public Affairs at Washington University School of Medicine in St. Louis.
Transcript
[music plays]
Jim Dryden (host): Hello. And welcome to “Show Me the Science,” a podcast about the research, teaching and patient care, as well as the students, staff, and faculty at Washington University School of Medicine in St. Louis, Missouri, the Show Me State. My name is Jim Dryden, and I’m your host this week. We’ve been focusing these podcasts on the COVID-19 pandemic and Washington University’s response. This week we’re speaking with Michael Avidan, an anesthesiologist and the leader of an international clinical trial that is launching to test the effectiveness of the malaria drug chloroquine. But this study won’t focus on sick patients. Instead, the goal is to determine whether chloroquine can protect front-line health-care workers. Avidan and his collaborators around the world are studying whether low doses of chloroquine might prevent COVID-19 infections in health-care workers, or, if they do become infected, keep those infections as mild as possible. And the global reach of the study is key, he says, because COVID-19 is a global pandemic.
Michael Avidan, MD: If it’s raging all around the world, it will keep coming back. So we have to address this problem on a global scale. This is a common enemy to all of humanity. Now more than ever we, as human beings, need to unite. We’re all in this together.
Dryden: Avidan is collaborating with scientists in the United Kingdom, southern Africa, central Africa, Ireland and Canada to protect those workers in a study supported by the COVID-19 Therapeutics Accelerator, a program designed to speed up the response to the pandemic by funding the identification, assessment, development and scale-up of potential treatments.
Avidan: There are three big things that we have to focus on. The first is testing. We need to figure out how extensive this pandemic is. The second is treatment. We have to do whatever we can to prevent people from getting COVID-19 and to treat them so that it doesn’t become severe. And of course, the ultimate solution is a vaccine, doing something that will stop it dead in its tracks. And what the Therapeutics Accelerator is focusing on is that middle pillar. And what is the Therapeutics Accelerator? It is a collaboration among various philanthropic organizations, including the Bill & Melinda Gates Foundation, MasterCard, and the Wellcome Trust, as well as other philanthropic organizations and individuals. And to distill its key aim into one sentence: Its goal is to identify potential treatments for COVID-19, to accelerate their development, and to prepare for the manufacture of millions of doses for worldwide use. And one of the drugs that has a lot of promise is the antimalarial drug chloroquine, which has been in use since the 1930s, has been administered to more human beings than virtually any other drug on this planet. We’ve got an extensive experience with this drug. It has a long track record of safety. We’ve used it for prevention of malaria, for treatment of malaria.
Dryden: Why are you focusing this particular study on health-care workers?
Avidan: So, health-care workers have a high incidence of severe COVID-19. And this is for several reasons. First of all, we tend to be exposed repeatedly to people who are infected with SARS-coronavirus-2.
Dryden: That’s the virus that causes COVID-19 infections.
Avidan: And often, when we become infected, we receive a high dose of the virus because we are dealing with people who are severely ill and who themselves have a lot of the virus on board when we interact with them. So if you’re a nurse or a respiratory therapist or a dietician or a cleaner in a hospital environment, you could become infected any time. An infection is insidious. It’s clandestine. Even if you’re thinking about a time of lockdown, when society is constrained, health-care workers are still coming into work on a daily basis. And in some countries, they’re using — in some cities, they’re using public transport. So there are also risks not just because of where they work, but because they’re unable to stay safely in their homes.
Dryden: So if chloroquine can effectively prevent infection or reduce the severity of the illness, are you saying it could be sort of like gloves or a mask, part of a health-care worker’s PPE?
Avidan: I entirely agree with what you’ve said, Jim. I think that thinking about this as part of our protective armamentarium. It’s not going to eradicate this. If it works, it will be a bit helpful, and it will complement, it will assist the other means we have of decreasing the devastation caused by SARS-coronavirus-2. So there are lots of things that we do. Physical distancing, hand hygiene are extremely helpful. And other things we do, like gloves and masks in a health-care setting or even masks when we are walking around on the street. I think more and more people should be wearing masks.
Dryden: And it’s still true that when people travel to parts of Asia, Africa, South America, they may be advised to take chloroquine to prevent malaria. Is that why you’re sort of interested in this drug as a means to prevent and protect from COVID-19?
Avidan: So, the importance of repurposing drugs. When you’re dealing with a new pandemic, if you’re trying to develop drugs from nothing, when you don’t have anything that’s approved or is shown to be safe in humans, the time from development to rolling it out into clinical practice is many years. And with a pandemic like COVID-19, we don’t have the luxury of time. And fortunately, we do have some medicines that have activities against other infectious agents or that are useful not just for the indication for which they were developed. Chloroquine is one of these, but there are several other medications. So there are all sorts of drugs that could be explored. That’s the purpose behind the Therapeutics Accelerator. And chloroquine is a drug that is known to have various actions against viruses and has shown promise in preliminary trials in humans in China. And we think that because of its multiple potential beneficial actions against SARS-coronavirus-2 it is one drug that really should be carefully explored in rigorously designed trials.
Dryden: Recently there have been studies saying that chloroquine may not be as effective as had been hoped. I understand that these aren’t controlled trials like you are designing here, but have they had an effect on your viewpoint, on your optimism, as you get set to begin this clinical trial?
Avidan: I want to answer by saying this has not changed my perspectives at all. I understand that all drugs can be dangerous when you use them inappropriately, when you give too much, or when you give them to the wrong people. And we know this. If drugs like chloroquine, or any other drug, that if you take in excess there can be real problems. The trials that you referred to, Jim, have used these types of drugs often in combination with other drugs where the safety of that combination isn’t very clear. And they also, by the way, they were using dosages of that drug which are equivalent to six times, six times the highest dose that we are using in our highest dose regimen. The other point is that if you give these drugs to people who are sick, who have heart disease, yes, then there is potential danger. But if you give these drugs at safe established dosages, which we are doing, to healthy people who don’t have diseases that make them at higher risk, like kidney disease, liver disease, heart disease.
So I think you have the problem here that these drugs are getting a bad reputation because they’re being given to people who shouldn’t be receiving these drugs. And also the settings within which there have been some of these concerns have been in people with very severe COVID-19 who are critically ill. We are giving these drugs to well-informed health-care workers who are healthy, and our purpose in doing this is to prevent people from getting COVID-19 or from getting serious COVID-19. And one of the concerns I have is that if you have a small trial that’s not rigorously designed, which doesn’t find that this drug works, it could be discarded prematurely.
Dryden: Talk about the dosage in this study. Because one of the goals is to protect health-care workers, but the other goal is to do it with the lowest dose of the drug possible.
Avidan: The reason that the lowest dose is so important is that if you think about any medication, any medication has side effects, and those side effects often relate to the dose that you give. The more you give, the more likely you are to experience side effects. The same is true of chloroquine. And many of the studies that have been done and have found safety concerns to date have used doses that are much higher than the doses that we’re using in this trial. We’re choosing three dose schedules in this trial. All of which are very well-established, all of which are very safe, and all of which have been used in thousands and thousands of people for many, many years. The value of figuring out the lowest effective dose is, first of all, you’ll have fewer side effects. And the side effects with a drug like chloroquine include itching of the skin, nausea, diarrhea. These are some of the problems that you have. And the more of the drug you take, the more likely you are to experience these side effects. And if you take a very low dose, really these side effects are very uncommon. But the other important point is if you think just about health-care workers, there are over 60 million health-care workers in the world. And if you think of other people who are at risk or even the whole world’s population, you’ll need millions and millions of dosages of this drug if you want to roll it out for people who are at risk.
Dryden: I’m wondering if part of what inspired you to want to do a worldwide trial like this is your background. Growing up training in South Africa and England. Does that give you, as you think about this, more of a worldwide approach to the problem of protecting these health-care workers.
Avidan: I grew up in South Africa. Definitely, my heart is in Africa. I have a real love for South Africa. And southern Africa, I’ve visited many countries there. I go back every year. When I was a young doctor, it was in the late 1980s and early 1990s, and I remember my despair with the HIV pandemic that was sweeping the world at the time, and seeing young people who were cut down by this devastating infection was very hard for me as a young doctor. And I also saw that the devastation wrought in Africa was very different from that in countries which had much better resources. And even today, the prevalence of HIV in South Africa is still about 25%. And where we, in more economically advantaged countries, have different health-care problems, the problems of infectious diseases are substantial in low- and middle-income countries in Africa, in Asia, in South America.
You also need to recognize that a pandemic like COVID-19 – this is a global village. We’re all in this together. You can’t eradicate COVID-19 in the United States alone. If it’s raging all around the world, it will keep coming back. So even from a selfish point of view, we have to address this problem on a global scale. This is a common enemy to all of humanity. Now more than ever we, as human beings, need to unite.
I want to stress that this isn’t research we’re just doing in Africa. We’re doing it in Africa and in Canada and in Ireland and in the U.K. It’s all collaborative. And we’re doing the same research throughout the world. We’re all in this together. But I think that Africa still remains an important focus because people there are extremely vulnerable. COVID-19 has the potential to cause real devastation in Africa. There are few health-care workers within Africa, and per capita, substantially fewer than there are in a country like the United States. Those health-care workers have less access to personal protective equipment than I do, for example, and I’m aware of that. All of these countries could be extremely vulnerable. And if the health-care workers are incapacitated, the health-care systems there will crumble.
When we help our neighbor, we help ourselves. There is no room with COVID-19 for division within society. It doesn’t matter if I agree with you, whether I disagree with you; if I like you or I dislike you. Keeping you safe keeps me safe. Keeping a different country safe keeps our country safe.
Dryden: Tell me where this all came from. What was the seed, the genesis of this whole thing?
Avidan: So the genesis of this was earlier in this year, we had a conference in South Africa, and we had investigators from all around the world and from various countries in the African continent. And we were seeing early on in this year the emergence of this pandemic. And we thought then, we really need to establish this worldwide network, where we could work collaboratively in a unified way to try to combat this virus. And I hope that when we as humans confront crises like COVID-19 that it brings out the best in us and that it allows us to find common cause in fighting a common enemy because, surely, there are major challenges that are posed by COVID-19. And so let’s use that to bring out some things that are good. And that after we’ve defeated COVID-19 that the world is a better place in some way. And we’ve used it to improve our society and the way that we all work together. It is such a critically important simple point that is easily lost. You cannot protect one country if you’re not protecting the whole world.
Dryden: And it’s hard to protect anyone if you don’t have enough health-care workers to care for them because the workers have gotten sick with the virus. Avidan says an estimated 30,000 such workers from across the globe will take various doses of chloroquine or inactive placebo. As the study progresses over several weeks, if the investigators find that a particular dose of the drug seems to be the most effective at protecting health-care workers, all participants will be able to receive that dose. Ultimately, the scientists want to identify the lowest dose of medication that provides the most protection for front-line health-care workers. The study will last for five months.
Show Me the Science is a production of the Office of Medical Public Affairs at Washington University School of Medicine in St. Louis. The goal of this project is to keep you informed and maybe teach you some things that will give you hope. Thanks for tuning in. I’m Jim Dryden. Stay safe.







