Podcast: Facing another pandemic holiday season
This episode of 'Show Me the Science' features doctors who face exhaustion as they work in emergency rooms and ICUs again crowded with COVID-19 patients
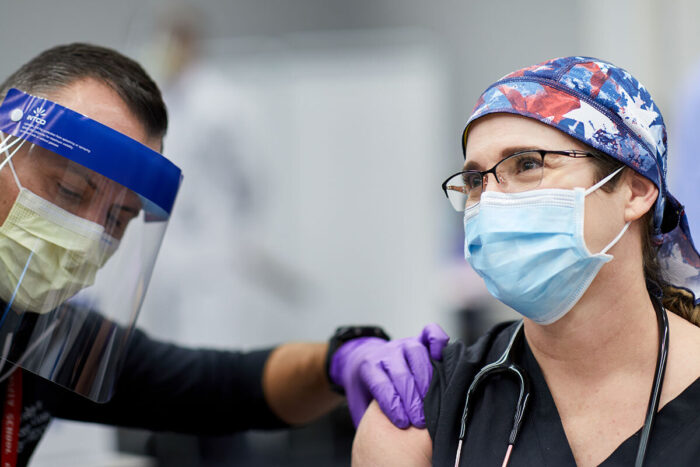 Matt Miller
Matt MillerTiffany M. Osborn, MD, a professor of surgery and of emergency medicine (right) receives a COVID-19 vaccination shortly after vaccines became available in late 2020. Now, a year later, as a second pandemic Christmas season arrives, Osborn and other Washington University physicians say they're tired, but they remain committed to taking care of the patients with COVID-19 who continue to arrive in the emergency department and intensive care unit.
A new episode of our podcast, “Show Me the Science,” has been posted. At present, these podcast episodes are highlighting research and patient care on the Washington University Medical Campus as our scientists and clinicians confront the COVID-19 pandemic.
The omicron variant of SARS-CoV-2 is here, but it’s the delta variant that has been driving a rapid increase in COVID-19 hospitalizations in recent weeks as people get out into the world more, antibody responses from vaccines wane, and families travel and gather in larger groups. As cases surge and hospitalizations increase, health-care workers are facing a second holiday season with emergency rooms and intensive care units (ICUs) crowded with COVID-19 patients. Nguyet Nguyen, MD, an assistant professor of medicine in the Division of Pulmonary & Critical Care Medicine, spent Christmas Day 2020 in the ICU. At the time, she hoped that what were then newly available vaccines would make 2021 markedly better. As she works with COVID-19 patients this year, Nguyen says she is doing her best to convince them and their family members to get vaccinated. Meanwhile, Tiffany M. Osborn, MD, a professor of surgery and of emergency medicine, says that although she and her colleagues are tired, they’re still committed to working hard to give patients what they need to get better. She says if more people could see what she sees, she’s convinced almost everyone would get vaccinated and wear a mask. For now, both Nguyen and Osborn say that they, unfortunately, expect to remain busy for the foreseeable future.
The podcast, “Show Me the Science,” is produced by the Office of Medical Public Affairs at Washington University School of Medicine in St. Louis.
Transcript
Jim Dryden (host): Hello and welcome to “Show Me the Science,” conversations about science and health with the people of Washington University School of Medicine in St. Louis, Missouri … the Show-Me state. As we continue to detail Washington University’s response to the COVID-19 pandemic, in this episode, we mark a grim milestone as the death toll in the U.S. from COVID-19 passes 800,000 Americans. And we speak with two Washington University physicians who have spent much of the last two years working with COVID patients in the emergency room and the intensive care unit at the medical school’s academic teaching hospital Barnes-Jewish Hospital in St. Louis. For the second holiday season in a row, the number of people in the hospital is rising, and that’s expected to continue. Dr. Nguyet Nguyen spent last Christmas Day working with COVID patients in the intensive care unit, and at that time she thought that the emergence of vaccines would make this year different. It didn’t. The delta variant has caused a rise in infections as the country opened up in recent months and as people have traveled to see family in recent weeks. Now, the new and potentially more infectious omicron variant has arrived, and for the second December in a row, hospitals are expecting a rapid rise in cases. Dr. Tiffany Osborn, who works in the ICU and the emergency department, says she has seen and continues to see a lot of people with COVID-19.
Tiffany M. Osborn, MD: You still have health-care workers who are committed to standing shoulder to shoulder to do what’s necessary to take care of our community, whatever that looks like. And on the other side of the coin, you have people who’ve been doing this for a really long time, and we are getting tired.
Dryden: Osborn and Nguyen are among the thousands of health-care workers who have spent a big chunk of their time since March of 2020 working with COVID-19 patients, and Nguyen says it’s tiring. She says she’s sometimes frustrated, but her job, she says, is to treat people when they get to the intensive care unit.
Nguyet Nguyen, MD: By the time the patient arrives to the medical intensive care unit, it’s too late for us to change what has already happened. So as physicians and as a medical ICU team, we do what we need to do to try to get them better. And then we look for opportunities to speak with their family regarding things like taking the COVID vaccine, taking the COVID booster. I always try to do my part to try to increase the rate of vaccination because I feel that that’s how we’re going to get through this problem. The vaccine works, and I try to promote vaccination of as many people as possible. There was one particular patient who most of his family members were vaccinated and he did not get vaccinated, and he had his several weeks’ stay with us. But he did get better and near the end, his wife was in the room and the subject of vaccination did come up, and he expressed a lot of reservations about the vaccine. So that was my opportunity to tell him about the vaccine and answer his questions, and he seemed to consider that. And then a few days later, his wife told me, and she was very happy and very thankful that he decided to get the vaccine before he leaves the hospital. So he got COVID, but my conversation with him, I was able to change his mind about getting the vaccine.
Dryden: Case numbers are up again the last few weeks. Delta is still the culprit here. It sort of robbed us of what we thought looked like it was going to be a normal summer and fall. Now we hear about omicron, a variant that appears to be even more transmissible than delta. Are you getting tired? You’re sort of looking into the future and knowing what could be ahead of us.
Nguyen: We are tired of COVID, but I realize and many of us realize that COVID is not going to be something that’s going to go away easily. So we need to hunker down and deal with it, with whatever variant that’s going to come along. So yes, delta was very deadly, and omicron is coming or omicron is here. Hopefully, it won’t be as deadly. And I think with the way things are going, I would anticipate that we’ll get other variants down the line. So, yeah, this is not something that’s going to go away. So in order to deal with that, we just need to resign ourselves to the fact that this is how life is going to be.
Dryden: What are your feelings this year compared to last year at this time?
Nguyen: So last year at this time, I was feeling pretty optimistic that the vaccination was going to be here, that 2021 was going to be a good year where we can get more protection for everyone and that things can “return to normal.” Now I know that things really can’t return to normal. It’ll be a different normal, but things will never be the way that it was. And then my outlook for 2022 is certainly not as optimistic as it has been for 2021, given what’s happened this past year regarding people’s reluctance with vaccination. And regarding the emergence of the delta variant and now the omicron variant, I really only see one way out of this, and many people are resistant to taking it that way. So I’m very sad for our country.
Dryden: Is it a different feeling now, knowing that you have more that you can offer to a patient, potentially? Or by the time a patient is sick enough to get to you, are your tools pretty much the same: helping them breathe or putting them on their stomach or whatever those tools are?
Nguyen: So we’re still with the same armamentarium that we had before, with mechanical ventilation, with prone position, with the supportive care that we’ve been giving the patient. On the brighter side, we’re more familiar with COVID, and we are more — not exactly comfortable, but we’re not as scared of COVID as we used to be. Treatment of the COVID patient has become a little bit more standard. Prior to COVID, we always had people that were sick every year with influenza. Now with the flu, we never had to have so many people get those extraordinary measures that we give for people with COVID.
Dryden: I’m imagining that before the pandemic, in the intensive care unit, whenever you’d have your team meeting or whatever before beginning care, you’d look and say, “Oh, this patient has this, and this patient has this, and, you know, here’s a heart problem, and here’s pneumonia.” How often do you come to work and see on your list of patients that they all have the same thing? That they all have COVID?
Nguyen: Well, I have been doing this for over 20 years. We don’t get eight to 10 to 12 to 14 people out of 17 with the same problem. So it’s very disheartening that despite having the monoclonals, despite having the vaccine, we’re still treating the number of people that we’re treating for an illness that, for the most part, is preventable in immunocompetent people. So it is a tragedy. We’re extremely frustrated with the ongoing debates about the vaccine. For us, it’s not a debate. There are people dying in our ICUs that it does not have to be that way.
Dryden: Numbers are up, probably because a lot of people traveled and got together at Thanksgiving time. And I’m imagining a lot of people are getting ready to travel and get together again at Christmas time and New Year’s and all through this holiday season. What are you going to do? How do you try in your personal life to stay as safe as you can around these holidays where, I mean, let’s face it, people want to see their loved ones. Can they do that safely?
Nguyen: Can they do that safely? It depends on what your definition of safe is. There’s ways to do it as safe as possible, but there is no way that humans can get together and be guaranteed that you’re not going to get exposed to COVID. And I understand people want to see their family. People need to see their family. I do come from a large family. Last year, I worked the COVID ICU on Christmas because my family is not in town. I did the Christmas shift to help out my colleagues whose family are in town so that they can enjoy their time with their family. But this year, I’m planning on traveling to visit with my family in Southern California. Every single one of my family members has been fully vaccinated. We plan to spend as much time outdoors as possible. I don’t think it’s reasonable to expect people to not travel and stay cooped up in their home. But if you are traveling, then please get yourself vaccines and booster and wear masks when you’re in a public area.
Dryden: A lot of that is the same advice we’ve been hearing for almost two years now. Dr. Tiffany Osborn says it’s hard for her to put her feelings about the situation into words.
Osborn: It’s an easy question. It’s a complex answer. You’re sort of looking for the monolithic answer of, “Everything is fine.” And on one side of the coin, you still have health-care workers who are committed to standing shoulder to shoulder to do what’s necessary to take care of our community, whatever that looks like. And on the other side of the coin, you have people who’ve been doing this for a really long time, and we are getting tired. We’ve been getting tired. I guess I would say that everybody is committed to patient care, and I have to still acknowledge that we are all trying our best in difficult situations.
Dryden: Last year at this time, the first people were just getting vaccinated. There wasn’t a way to prevent some of this, and I know there are breakthroughs. And with omicron coming, there’s probably going to be more breakthroughs. Does that make things feel different from the point of view of health-care providers like you?
Osborn: So again, it’s sort of a complex answer. But what I would say is that overall, I’m going to say, no, it doesn’t make a difference when we’re treating people individually, right? Because our job is to meet you where you are. The other side of the coin is it’s frustrating because there are things that you can do to help mitigate that risk to yourself and to other people. That is frustrating, but I think that’s frustrating to a lot of people in the general community. But when it comes to how we do our job, the way we do our job, when we do our job, how we do our job — that commitment is still there. We still do everything that we need to do to take care of people when they need it, where they need it and how they need it.
Dryden: I remember thinking in March of 2020, “What will I do if this lasts all the way until the Fourth of July?” And now, here we are coming up on two years. Had someone told me then it was going to be at least two years, I would have set my hair on fire or something. I’m wondering, as you continue to show up for work, you continue to provide care — but had you known on the front end that we were going to be here now, what would your reaction have been?
Osborn: I think what I can tell you is that I’m glad that I didn’t know that then. Not because it would change how we do things. I think that when you’re faced with a pandemic that we haven’t dealt with in our lifetimes … yeah, I’m glad I didn’t know at the beginning how long this was going to last. But the other issue to this is that how long it lasts is really, in many ways, based on what we do to prevent it, because every time someone gets an infection, they get the potential for the virus to mutate, which is what we’re seeing right now with omicron. The longer the virus goes on, the more opportunity there is for it to continue to mutate.
Dryden: Without betraying any doctor-patient confidentiality, are there any cases that you’ve dealt with recently or since the beginning of this that just stick out in your head as sort of, “This is what I’m going to remember about COVID?”
Osborn: The day that I think of — and this was actually when we were just starting to have the opportunity to get the vaccine, so people didn’t have the vaccines yet — that was on January 6. I have several patients, and one of them in particular, every day I would go in, and he’d say, “How am I doing, Doc?” And I’d say, “You’re the healthiest person I have in the ICU right now.” And he was. Until he wasn’t. But I can remember sort of being there and being called into his room right after we had lost somebody else. And he was holding my hand, and I said, “It’s OK. We’re going to need to give you the breathing tube like we talked could potentially come.” And he was, of course, worried, and I was telling him, “No. I know you’re concerned, but we’re right here, and we’re going to take care of you.” We intubated him. And then next door to him was another person who, he wasn’t going to survive. And you’re about to leave the room, and you hear him on the phone. Yeah, he was on the phone. You hear this little voice come across. And he says, “I love you, Grandpa.” As you’re walking out the room and you just think you go from there to another room with someone who’s doing OK and you get to say, she says, “How am I doing, Doc?” And you say, “You’re the healthiest person in my unit right now,” because the one who was no longer is. Every single one of the people that I just talked about didn’t make it out of the hospital.
Dryden: That does bring up the question. We have passed 800,000 deaths in our country. How does that make you feel?
Osborn: Well, I’ll tell you that it’s not just the medical community that’s dealing with the responses. It’s all of us. You just don’t realize it yet. I think what we as a community need to understand is that our resources are limited. And so I guess what I’m getting at is that we all need to do our part, whatever we can do to mitigate the potential risk of contracting this illness and having to be in the hospital — that’s not only taking care of you, but it’s taking care of the community. So often you hear this question that, “If I make this decision, then I’m the one who reaps the consequences from it.” And the answer is that it’s not true. I guess the point that I’m trying to make is that what we do impacts each other. We’re a community. We should be working together to try to get through this in the best possible way. And the best possible way may not be the optimal way, but at least we’re looking out for each other.
Dryden: How are you going to spend the holidays? Will you be working? Will you have a big family gathering? How do you stay safe? How do you do your part? Obviously, you’re doing your part when you’re on the unit and you’re helping people. But outside, I mean, what decisions are you making about this holiday?
Osborn: We’re going to be staying – luckily, I actually have Christmas off this year. So my family and I are going to be staying together. It’s just going to be my immediate family. But what we do is we make sure we’re vaccinated. And when we met some of our extended family over Thanksgiving, everybody had to be vaccinated. And getting the booster. I’ve already got the booster. My husband’s got the booster. My daughter’s got the booster. Now we’re looking at my son. So I think the way to do your part is, one, from a medical standpoint, which is when you’re out in public, wear a mask. From a personal standpoint, you and your family get vaccinated and get a booster. And then from a community standpoint, look out for your neighbors, and make sure that your neighbors have what they need.
Dryden: Osborn and Nguyen both say they expect the number of COVID-19 patients in the hospital is going to rise again pretty significantly as we head into 2022. But both still say they have hope that at some point in the not too distant future, our lives and theirs might return to being more like they were before any of us ever heard of SARS-CoV-2.
“Show Me the Science” is a production of the Office of Medical Public Affairs at Washington University School of Medicine in St. Louis. The goal of this project is to keep you informed and maybe teach you some things that will give you hope. If you’ve enjoyed what you’ve heard, please remember to subscribe and tell your friends. Thanks for tuning in. I’m Jim Dryden. Stay safe.







