Podcast: As ‘Show Me the Science’ turns 2, we look back at 2 years of a pandemic
This episode of 'Show Me the Science' focuses on what was learned and what science got right and wrong about COVID-19
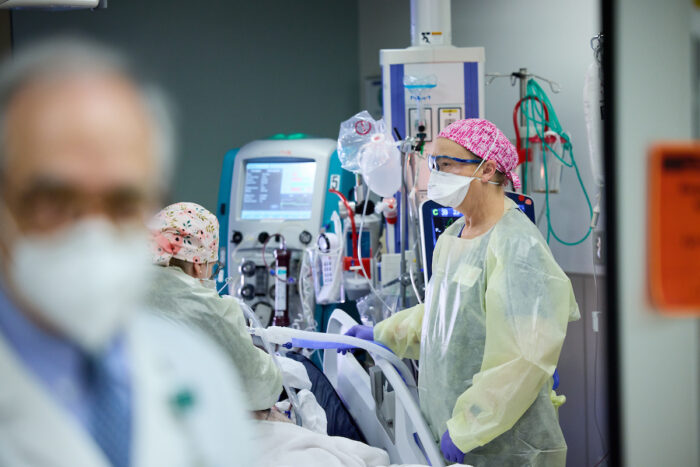 Matt Miller
Matt MillerA care team works with a patient in the intensive care unit at Barnes-Jewish Hospital during the COVID-19 pandemic, a common scene over the past two years. In this episode of "Show Me the Science," infectious diseases specialist Steven J. Lawrence, MD, looks back and forward, detailing some of the frustrations, surprises and successes of the past two years as we begin a third year of life in a pandemic.
A new episode of our podcast, “Show Me the Science,” has been posted. During the first two years of COVID-19, these episodes have highlighted research and patient care on the Washington University Medical Campus as our scientists and clinicians confront the pandemic. As we begin a third year of podcasts, we plan to expand our scope to include stories of other groundbreaking research, as well as lifesaving and just plain cool work being done by faculty, staff and students at the School of Medicine.

But for this episode, we’re sticking with COVID-19. In 2020, when the pandemic shut down much of the country, our very first guest on “Show Me the Science” was Steven J. Lawrence, MD, a professor of medicine in the Division of Infectious Diseases. He also was our first guest of our second season of podcast episodes last year. And we’ve brought him back again, for year three.
As the pandemic first gripped the St. Louis area, Lawrence was worried whether there would be adequate ventilators, ICU beds and medical staff to care for patients with COVID-19. A year later, in spring 2021, he was touting vaccines as a potential way out of the pandemic. Now, after having to deal with the delta and omicron variants of the virus, and with new worries about an even more infectious version of omicron, Lawrence has thoughts on moving forward as well as what people got right and wrong during the first two years of the pandemic. He also has some ideas regarding where we may be headed.
The podcast, “Show Me the Science,” is produced by the Office of Medical Public Affairs at Washington University School of Medicine in St. Louis.
Transcript
Jim Dryden (host): Hello and welcome to “Show Me the Science,” conversations about science and health with the people of Washington University School of Medicine in St. Louis, Missouri … the Show-Me State. During the two years we’ve been producing this podcast, we focused entirely on the way our doctors, researchers and trainees have responded to the COVID-19 pandemic. Now, as the pandemic, we hope, begins to recede, we plan to bring you stories of other groundbreaking research, lifesaving and just plain cool work at the School of Medicine. But for this, our first episode of our third season, we go back to COVID. Our very first guest when this podcast launched in 2020 was infectious disease specialist Dr. Steven Lawrence. The first time we spoke, emergency rooms were crowded, and office buildings were starting to empty as workers who could do their jobs from home were encouraged to stay there. Lawrence says doctors and scientists have learned quite a bit about the virus during the last two years. During that time, the various strains of the virus contributed to more than 6 million deaths around the world, with more than a million of those in the United States, numbers higher than even most worst-case scenarios when the virus first appeared in 2020.
Steven J. Lawrence, MD: The virus hasn’t behaved like we would have initially predicted. And as we learn more, we learn that initial assumptions may not have been accurate and that you update those. This is the way science works. This is the way medicine works.
Dryden: We sat down with Dr. Lawrence again recently to talk about how science and medicine have adjusted and been updated since the first time we spoke about COVID-19 almost exactly two years ago.
Lawrence: It is a little depressing that we’re still having to think about and talk about this COVID pandemic on an almost daily basis two years into this. But every day, still, there are new things that we’ve learned, new developments, new changes, that really require us who are involved with this response to really pay attention to even almost daily changes.
Dryden: So two years ago, in that very first episode, you said, and I quote, “If this virus acts like most respiratory viruses, you would expect …”
Lawrence (in 2020): If this virus acts like most respiratory viruses, people who are infected during this wave will be protected for future waves, particularly ones in the near future because then we have what’s called herd immunity. And ultimately, when we do have enough people who are immune …
Dryden: So I ask, are what we’re seeing is a virus that doesn’t act like most other respiratory viruses? Is it a case where even with around 500 million infections around the world, we’re not yet at herd immunity? Or has herd immunity ceased to be a useful concept when it comes to SARS-CoV-2?
Lawrence: I think we were partly right with that description of how this virus might behave. And there’s no doubt that prior infection does provide meaningful and important protection for individuals. What has emerged are a couple of things. First, the degree of protection is not adequate in most cases, especially milder cases, to be able to prevent reinfection. However, there is some evidence that just like with vaccines, even if the protection versus infection wanes over time, there is still meaningful and significant protection versus serious disease. It does, with new variants, certainly have the ability to evade the immune response that was generated from prior variants, but not enough to still then start from scratch as far as protection versus getting really, really sick. And I think omicron displayed this more than anything else. People who’d been infected with a prior variant, including even delta, did not have a large degree of protection versus becoming infected with omicron. And so there was a huge surge. And yet, despite the huge numbers of actual infections, the hospitalizations were lower than what we saw during delta. And I think this is partly reflected by some evidence that omicron itself isn’t quite as virulent as delta. But probably more importantly is that, by that point in time when omicron hit, a pretty large percentage of the population had been infected or vaccinated already, and when they have a breakthrough infection or reinfection, it’s less likely to be severe.
Dryden: You also were the first guest as we started our second year on this podcast. And at that point, the news was that vaccines were becoming more widely available. And you thought perhaps the vaccine story was going to be what you called a public health triumph, both because it was produced so quickly and because it was so effective.
Lawrence (in 2021): The vaccine story is going to be one of the world’s greatest public health triumphs. That you went from the worst pandemic in 100 years, a novel virus that had never been seen before, and within 12 months, we went from the first cases being identified to having a vaccine that is safe, it’s effective, and it is not, I believe at this point, an exaggeration to say that they are the game changers that will allow us to put this pandemic in the rearview mirror.
Dryden: But then came delta and omicron. Is it still in your mind a public health triumph, or maybe tempered a little bit by what happened in the last year?
Lawrence: There’s no question the COVID vaccines and the campaigns to produce them were a real triumph and that there have been millions of lives saved across the globe and hundreds of thousands already in the United States because of the vaccines. A year ago, we were looking at and using the phenomenal data that emerged from the clinical trials that showed that the, especially mRNA, vaccines prevented any infection with 95% effectiveness. What emerged after about six months after the vaccines became widely available is evidence that clearly showed waning of immunity versus at least mild infection. But very importantly, the vaccines still do the most important thing, which is prevent serious illness.
Dryden: Which brings us to the relatively new news that some older Americans now are able to get another booster if they choose to. What’s the reasoning behind that?
Lawrence: Yeah, the reasoning behind all of the vaccine decisions that are made as far as who should be getting what and when are really based around trying to prevent severe illness and hospitalizations. Omicron really has changed the paradigm in how we’re thinking about COVID because of the fact that when you have a variant that emerges that is so contagious and can evade immunity from prior infection or vaccination — again, to get infected — but it causes milder disease, the goals had to change somewhat. And that goal is preventing serious illness. And that is where the recommendations now are really tied towards. Age 50 and older is a very broad range. Somebody who is 50 and healthy with no other medical conditions compared to somebody who is 75 or 80 with diabetes and cancer, the relative need is certainly higher in those who are on the higher risk end of the spectrum.
Dryden: Masks are going away. You see big crowds at concerts, indoor sporting events, theaters, symphony halls. They’re all reopening. So I’m wondering if this is a recipe for another surge.
Lawrence: We are at levels of transmission in the community that are as low or lower than we’ve seen in two years since the pandemic started, which has meant that it is a reasonable time during this lull in activity that the relaxation of the mitigation measures and masking, in particular, is reasonable because we are very likely to need to pull that out of our toolbox again when there are significant rises, especially if there are rises that lead to any potential strain on our health-care system. And so the combination of this new subvariant and with a relaxation is likely to cause some increase. That’s an increase from historically low levels, and so even a doubling or a tripling in the case rates in the short term would not lead to a serious public health crisis of overwhelming our health-care systems. But we do have to watch carefully because, again, we just don’t know if the potential is there to see rapid rises and a surge that would be similar to either delta or omicron like we saw, or if it would be much smaller.
Dryden: You and I have discussed, pretty much every time we’ve spoken over the last two years, as long ago as March of 2020, you were worried that the health-care system might even collapse under the weight of this virus. And that was long before the subsequent waves, particularly omicron, which hospitalized significantly more people. Even though it may have been milder in most people who were vaccinated or previously infected, when I would see the numbers of patients, it was, “Holy cow!” How would you rate the relative health of the system after two years under this weight of COVID-19?
Lawrence: Well, I think there have been certainly a lot of things learned and that there is resilience in the health-care system to be able to figure out how to absorb a large number of patients that may not have been possible when it first hit in March of 2020. The delta surge, in particular, is what was the major strain on our health-care systems to the point where we were very close to collapse. And if it had gone another week or two of rising, before the peak occurred, it may have actually been a point where if a person has a heart attack or a car accident, that they may not be able to receive lifesaving care that they need because the hospitals are too full. And part of the resiliency that has developed is, one, finding out how we can take care of patients in different places in the hospital on different wards. Fortunately, there’s been a little bit of a pattern change. When omicron hit, while the hospital numbers were still actually quite high, there weren’t quite as many of the patients who needed critical care. It takes many more resources to care for critically ill patients. And so we’ve been able to figure out ways to absorb a higher number, which can be more readily done when these are people hospitalized who may not be quite as sick. And, in fact, in a lot of instances, because there was just so much COVID during the omicron period, that many people who are hospitalized for other reasons also happened to have COVID even though they weren’t there because of the COVID.
Dryden: One of the things that I’ve heard in a lot of media reports is about messaging, that the COVID-19 messaging has been confusing. But as somebody who’s been listening to these messages from people like you and others, I wonder if that’s because not that the message was confusing, but that the situation was confusing. And the metaphor I’ve come up with is the Super Bowl. So if somebody’s watching the Super Bowl, and first, they said the Bengals were winning, and then they said the Rams won. I mean, can’t they make up their minds? Their messaging is inconsistent. So I don’t mean to be flip, but how much was problems with messaging, and how much was that the situation was fluid?
Lawrence: Well, certainly there are elements of both. The situation certainly has been fluid. We have been humbled in how much this virus has changed over time, how much we’ve learned from it. The virus hasn’t behaved like we would have initially predicted. So there certainly has been a lot of fluidity, a lot of change that was driven by the virus. And as we learn more, we learned that initial assumptions may not have been accurate and that you update those. This is the way science works. This is the way medicine works, is that you give an assessment of the best course of action based on the knowledge that you have at the time. And then you continuously review, and then you revise. In fact, it would have been not only negligence, it would have been a disaster if, for example, we all decided in the medical and scientific community that we’re going to stick to our original plan and answers just so we don’t sound like we don’t know what we’re talking about, and who cares what the results will be? And that would be so irresponsible. So what actually happens is that as you learn more, you say, “Hey, this is what we’ve learned. This is what’s different. This is what’s changed. And here’s how we enact it.” One of the pieces that’s really important with messaging — and some have done very well and others not so well, and I think I’ve been guilty of it myself sometimes — is to be careful not to sound too sure and too confident that this is what’s going to happen or that we have no humility that there’s a possibility that things could evolve and be different. So as long as we recognize that we are describing what is the best course of action based on the available data and that that can change, I think we’ll be OK. Now, this pandemic has had — there have been factors that have made the messaging far more difficult in that there have been intentional misinformation campaigns and intentional confusion being sown particularly around the effectiveness and relative risk to benefit of vaccines that have unfortunately led to confusion and perhaps lack of ability for everybody to be able to hear accurate information and make good decisions based on that information. COVID is going to be with us for the rest of our lives. It’s very likely. And again, as I just gave my own lesson here, I don’t want to make sure that we sound too sure of ourselves. But it’s likely that this is a virus that will establish itself as a permanent fixture in human experiences. We are still in a phase where it’s serious enough as a virus to be a very substantial risk for those who are older, for those who have compromised immune systems, and for those who haven’t been vaccinated or survived an infection yet. And so despite the fact that for the vast majority of people who get this virus infection is actually now relatively mild — and that is remarkably true and consistently true for those who are fully vaccinated and up to date on their vaccines — but we’re still not at a stage yet where there’s enough of a population that is protected to just treat this as a cold because there are still going to be, what I think most people in medicine believe to be, unacceptably high levels of people getting very sick and dying that we must not completely abandon, one, our ongoing need to make sure that as many people as possible, especially those at risk, are up-to-date with COVID vaccines; and two, to not be afraid to pull out and use those tools in our public health toolbox when we need them. Masking as a requirement has been one of the most controversial issues that has emerged throughout this pandemic. There are some factual components to it. This virus is a respiratory virus. It’s transmitted through the respiratory route. Masks, when they’re used, especially universal masking so that everybody is wearing them, have a marked difference. It has allowed most workplaces to be able to function with minimal, if any, transmission occurring in the workspace during even the peaks of delta and omicron. And that’s powerful because without those, we couldn’t have kept businesses running, couldn’t have kept kids in school. And we should not be afraid to use that tool again intermittently and on an as-needed basis moving forward. Nobody’s going to be harmed to say, “OK, for the next two weeks or three weeks, we’re going to all mask.” That can still allow for normal operations of workplaces and schools, and it will save lives. So these are tools that I think we should not be afraid to pull out and use again on just a temporary as-needed basis in the future.
Dryden: Will there be new treatments, perhaps different vaccines, new variants? If there are, future episodes of “Show Me the Science” will bring you information about them. We also know that as we launch season three of this podcast, the scope is going to expand beyond COVID-19, though I would predict that COVID-19 is still going to be discussed in this place a lot. “Show Me the Science” is a production of the Office of Medical Public Affairs at Washington University School of Medicine in St. Louis. The goal of this project is to introduce you to the groundbreaking research, lifesaving and just plain cool work being done by faculty, staff, and students at the School of Medicine. If you’ve enjoyed what you’ve heard, please remember to subscribe, and tell your friends. Thanks for tuning in. I’m Jim Dryden. Stay safe.







