New discovery could help improve cancer vaccines
Scientists identify key features of mutated tumor proteins vital for vaccine development
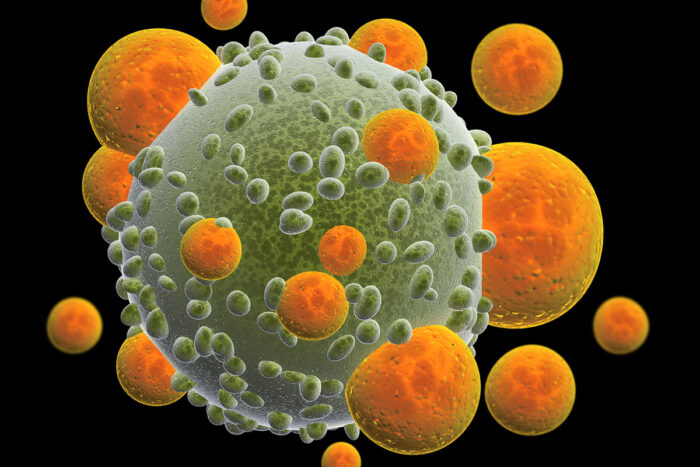 Getty Images
Getty ImagesShown is an artist's rendering of the immune system's T cells (orange) attacking a cancer cell. The mutated DNA of cancer cells often produces abnormal proteins, whose fragments can help distinguish the tumor from healthy tissue. New research — co-led by Washington University School of Medicine in St. Louis — has identified the most important features of the protein fragments to help researchers design better immunotherapies against cancer, including vaccines.
Cancer vaccines have shown promise in treating certain tumors, such as melanoma. But such vaccines have limitations. They often target normal proteins that may be more abundant in the tumor but also are present in healthy tissue, which can lead to off-target effects that cause autoimmune disorders and also reduce the effectiveness of the vaccines.
The mutated DNA of cancer cells often produces abnormal proteins, whose fragments can help distinguish the tumor from healthy tissue. Such protein fragments could be harnessed to train the immune system to attack the tumors with, in theory, few side effects. Now, a broad collaboration of scientists in academia and industry have identified the most important features of the protein fragments to help researchers design better immunotherapies against cancer.
The study, co-led by researchers at Washington University School of Medicine in St. Louis, appears Oct. 9 in the journal Cell.
These abnormal protein fragments are called neoantigens. The new study identifies five features of neoantigens that optimize the ability to trigger the body’s T cells to attack the cancer and leave healthy tissue untouched. Using the new criteria, the researchers used computer modeling to accurately predict 75% of effective neoantigens and eliminate 98% of ineffective mutant proteins in melanoma and a common type of lung cancer.
The research team, called the Tumor Neoantigen Selection Alliance (TESLA), has made the computer model and dataset freely available to the research community to speed the development of cancer vaccines and other immunotherapies.
“For scientists working to create personalized cancer vaccines that target the unique neoantigens of an individual patient’s tumor, this is a resource that is desperately needed,” said co-senior author Robert D. Schreiber, PhD, the Andrew M. Bursky & Jane M. Bursky Distinguished Professor of Pathology and Immunology. “There has been an explosion of approaches to try and figure out which are the best mutant proteins to target in a tumor. This broad approach is more accurate and will help to design anticancer vaccines that potentially are more effective for patients.”
The features that the researchers identified as most important in selecting effective neoantigens include the abundance of a specific neoantigen in the tumor; the strength with which the neoantigen binds to vital immune proteins so the T cells can see it; the stability of the neoantigen on the immune protein complex; how much more often the immune proteins preferentially bind to the neoantigen versus the normal protein; and how foreign or distinct the neoantigen is from the normal protein.
Schreiber said that all these factors make sense in selecting the best neoantigens, but he was surprised by some of the findings on criteria that were not important for neoantigen effectiveness.
“We were able to eliminate some of the assumptions that we scientists sometimes make about what makes a good neoantigen,” said Schreiber, who also directs the Andrew M. and Jane M. Bursky Center for Human Immunology & Immunotherapy Programs at Washington University School of Medicine. “For example, there has been a general sense that the mutant proteins that make the best neoantigens are the most hydrophobic — meaning they repel water. It turns out, that characteristic didn’t show any relationship to neoantigen effectiveness.”
Schreiber also pointed out that this study is focused on neoantigens that activate what are called CD8 T cells, which he describes as the immune system’s foot soldiers, those responsible for killing the tumor cell. He said future work should focus on neoantigens that also activate a different type of cell, CD4 T cells. Schreiber calls these the generals, cells that stay behind the front lines but direct the foot soldiers in their anti-cancer mission.
“In order to get a good immune response against a tumor, you need to activate both CD4 and CD8 T cells,” Schreiber said. “In future work, we would like to conduct a similar analysis to identify the best neoantigens for triggering the CD4 T cells as well. In designing an effective vaccine, we think we need at least one good CD8 neoantigen and one good CD4 neoantigen to trigger immune rejection of a tumor.”
The TESLA initiative, led by the Parker Institute for Cancer Immunotherapy and the Cancer Research Institute, includes 33 research teams from universities, biotech companies, pharmaceutical companies and nonprofit research institutes.







