Intraoperative imaging improves brain tumor removal
Using new versions of familiar technologies, Washington University surgeons are improving treatment of common brain tumors known as pituitary adenomas
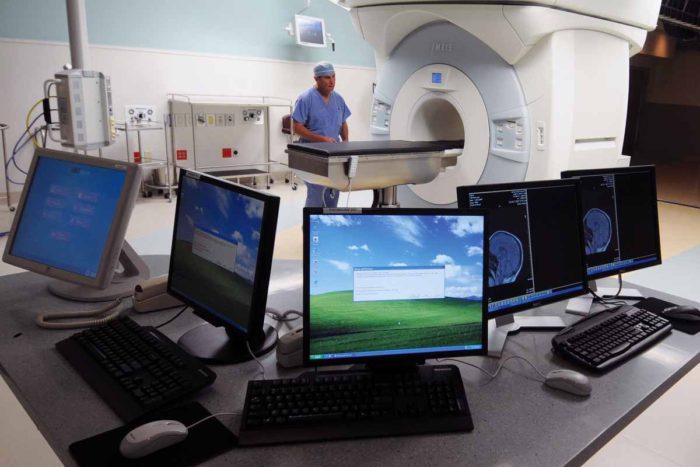
Room with iMRI equipment, which is used to help improve brain surgeries.
Surgeons are using new imaging technologies such as intraoperative MRI, or iMRI, in which an MRI unit is built right into a neurosurgical operating suite so that they can take scans and assess progress during surgery.
The technologies provide a level of detail previously unavailable in the operating room. And according to a recent study, the payoff is real: Surgeons remove tumors more completely during surgery, and patients have better outcomes afterward.
“In more than one-third of the cases where the iMRI was used, surgeons went back in to remove more tumor after the scan, and nearly 10 percent of these patients ended up with a more favorable level of tumor removal.” says Michael Chicoine, MD, the August A. Busch Jr. Distinguished Professor of Neurosurgery. “This should result in reduced need for additional surgeries, radiation treatments or other medical therapies after surgery, and decreased regrowth of tumors.”
Specially designed technology
The 6-ton iMRI unit is housed in a storage bay between two larger-than normal operating suites and moves on an overhead rail system. Because the iMRI device contains a large magnet, operating room personnel have to carefully remove all metal objects from specified areas of high magnetic fields—highlighted on the floor with painted labels—prior to its entry into the room. Once prepared, they can pull the iMRI into place in approximately 90 seconds to examine a patient during surgery. The surgical table and the mount, which holds the patient’s head, are specially designed and manufactured for iMRI compatibility.
The movable iMRI device installed at Barnes-Jewish Hospital in 2008 was among the earliest of such devices installed in the world; it has been used in more than 1,000 operations there—more than at any other hospital in the United States.
Neurosurgeons now have used the iMRI to check progress during surgery for both benign and malignant brain tumors and epilepsy, drainage of cysts, placement of catheters into the brain and many other procedures for both adult and pediatric patients.
The challenge of removing pituitary adenomas
Pituitary adenomas are typically benign tumors that occur in the pituitary gland, located at the base of the brain. They account for nine to 12 percent of all primary brain tumors—those that originate in the brain rather than spreading from other locations. The pituitary is often called the master gland because it strongly influences many important bodily functions, including growth, reproduction, blood pressure, metabolism and body temperature. Pituitary tumors can cause vision problems, headaches, depression and other psychiatric disorders, weight gain, facial disfigurement, and many other complications.
As with any surgery, physicians removing pituitary adenomas have to balance their goal of removing tumor against the need to minimize harm and loss of healthy tissue. Surgeons typically remove these tumors by performing surgery on the brain through the nose using endoscopes, instruments used to visualize inner body cavities. The latest generation of surgical endoscopes provides them with high-definition video images to visualize the tumor and the surrounding critical anatomy such as nearby arteries and nerves.
“We often get the endoscope very close to the site of the tumor and use it to make sure we’ve cleared the tumor cells,” Chicoine says. “And when we can’t get that close, there are features of this technology such as angled endoscope tips that let us do things like see around corners.”
Still, it sometimes can be difficult to distinguish between healthy tissue and tumors through visual inspection. The iMRI fills this need. With the aid of injected imaging agents, it provides a complete field of view with starker, more precise contrast between healthy tissue and tumor cells, helping surgeons determine whether any additional removal might be possible.
When feasible, maximal safe removal, of course, is the goal; patients with tumor remaining after surgery may need to undergo additional medical treatments, radiation treatments, or, in some cases, a second operation.
Better view, better results
A recent study by physicians from the Pituitary Center at Washington University shows that patients benefit from these advanced technologies during and after surgery. Lead author and neurosurgery resident Peter Sylvester, MD, analyzed data on 446 patients requiring pituitary adenoma surgery performed at Barnes-Jewish Hospital between 1998 and 2012. The iMRI was used in 156 of these cases.
Sylvester and collaborators found that in 35.9 percent of the iMRI cases, doctors were able to identify additional tumor and remove it.
To assess the long-term impact, Sylvester and his colleagues analyzed data from follow-up examinations in the months and years after surgery. They found that 9.6 percent of patients who received additional surgery after iMRI shifted toward a category of patients who are at lower risk for their cancer to recur. They also found that iMRI and endoscopy did not increase the post-surgical complication rate.
The results were published online in the journal Pituitary in March.
“The iMRI and our new endoscopes really impact what we do quite a bit,” says Chicoine. “They are amazing and enabling technologies, and we’re continuing to improve and expand our use of them.”
Dr. Chicoine has received an unrestricted educational grant from IMRIS, Inc., the corporation that manufactured and installed the movable iMRI device at Barnes-Jewish Hospital. This grant supports John Evans, RN a research nurse who maintains the intraoperative MRI and brain tumor databases in the Department of Neurosurgery at Washington University, and the IMRIS Multicenter Intraoperative MRI Neurosurgery Database (I-MiND) for which Dr. Chicoine and Washington University are the coordinating site for a multicenter collaborative project.







