International Alzheimer’s clinical trial to test two drugs in combination
Drugs targeting amyloid, tau to be evaluated together
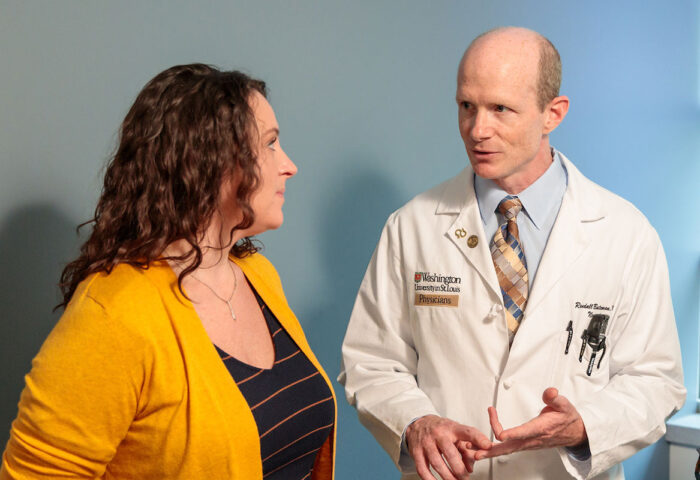 Matt Miller
Matt MillerTrial participant Rachel Habiger meets in 2018 with Randall J. Bateman, MD, the director of the Dominantly Inherited Alzheimer Network Trials Unit (DIAN-TU) at Washington University School of Medicine in St. Louis. The DIAN-TU has announced that it will be targeting two key Alzheimer’s proteins — amyloid and tau — as part of its Tau Next Generation Alzheimer’s prevention trial.
Researchers leading a worldwide clinical trial aimed at finding treatments for Alzheimer’s disease are modifying an arm of the trial to evaluate a combination of drugs targeting two brain proteins: amyloid and tau. The trial – known as the Tau Next Generation Trial (Tau NexGen) – originally was announced with a focus on drugs that target tau, but with increasing evidence that targeting amyloid can reduce biomarkers of Alzheimer’s disease, the trial’s leaders have revised the first arm to include an experimental therapy targeting amyloid as well.
Tau NexGen is part of the Dominantly Inherited Alzheimer Network Trials Unit (DIAN-TU), led by investigators at Washington University School of Medicine in St. Louis. The DIAN-TU is an international network of academic centers focused on finding therapies for Alzheimer’s disease by studying people who have rare, inherited mutations that almost certainly guarantee they will develop the disease at an early age.
“With growing evidence that removing amyloid plaques has biologically beneficial effects on amyloid and tau, we believe that targeting both Alzheimer’s disease pathologies — amyloid plaques and tau tangles — at the same time can provide the highest chance of success,” said principal investigator Randall J. Bateman, MD, director of DIAN-TU and the Charles F. and Joanne Knight Distinguished Professor of Neurology at Washington University.
The DIAN-TU launched in 2012 as the first prevention trial platform for Alzheimer’s disease. A trial platform allows multiple treatments to be evaluated using a single master protocol. The first therapies evaluated on the DIAN-TU platform were designed to target the buildup of amyloid plaques in the brain. Such plaques are thought to contribute to problems with memory and thinking. With the initiation of the Tau NexGen trial, the DIAN-TU has extended its focus to another Alzheimer’s disease pathology, tau tangles, that has been closely linked to cognitive decline.
The Tau NexGen trial is designed with three arms. Each arm will evaluate an investigational drug that targets tau; each drug is designed to work in different ways.
The first arm of the Tau NexGen trial will evaluate an experimental anti-amyloid drug called lecanemab (designed to target forms of amyloid called oligomers and protofibrils) and an investigational tau drug known as E2814 that is designed to target the spread of tau. Both drugs are developed by the Japanese pharmaceutical company Eisai Co., Ltd. This will be the first Alzheimer’s prevention trial to target both amyloid and tau with two drugs at the same time.
For the other two arms, the research team plans to choose from two classes of tau drugs that act in different ways: by targeting other mechanisms of tau pathology, including small molecule drugs that inhibit tau aggregation; and genetic treatments that reduce the production of tau protein. Future tau drug arms may also be combined with amyloid drugs such as lecanemab.
The Tau NexGen trial is primarily funded by the National Institute on Aging of the National Institutes of Health (NIH), with significant support from Eisai, as well as the Alzheimer’s Association and philanthropic donations. Eisai is contributing E2814 and lecanemab to the trial.
Earlier this year, DIAN-TU leaders announced that the first arm of Tau NexGen would evaluate the experimental tau drug E2814 alone. As the trial was still in the process of being launched when the design change was made, no participants had yet begun drug treatment under the tau-based protocol.
Under the revised protocol, all participants will receive the amyloid drug, while half also will receive the tau drug and half the placebo. The timing of each drug depends on whether the participant has begun experiencing cognitive changes. Symptomatic participants will receive the amyloid drug for six months before being randomly assigned to also receive the tau drug or a placebo. Since amyloid plaques accumulate before tau tangles in Alzheimer’s disease, this study design allows the researchers to assess whether amyloid removal clears the way for the tau drug to function most effectively.
At the same time, presymptomatic participants will be randomly assigned to receive the tau drug or a placebo for a year before beginning the amyloid drug. By staggering the drugs in this way, the researchers will be able to evaluate the effects of the tau drug alone before assessing the effects of the two drugs together.
The primary endpoint is a slowing of tau accumulation in the brain in symptomatic participants, as seen on PET brain scans. As a secondary endpoint, the researchers will evaluate whether the drugs affect levels of a specific kind of tau — phosphorylated tau 217 — in the cerebrospinal fluid of presymptomatic participants. Bateman and colleagues have shown that levels of phosphorylated tau 217 in the cerebrospinal fluid rise steadily as the disease silently advances before symptom onset. The researchers will assess whether drug treatment slows the rise in levels of this form of tau in the presymptomatic group.
If these primary and secondary endpoints are positive, the trial will be extended for another two years to assess whether the drug slows cognitive decline and has further effects on tau pathology.
The DIAN-TU trial platform is the first trial platform aimed at identifying drugs to prevent or slow Alzheimer’s in people who are nearly certain to develop the disease due to genetic mutations. People who inherit such mutations tend to develop symptoms at around the same age their affected parents did, often in their 50s, 40s or even 30s. While devastating for families, such mutations allow researchers to identify and study people in the earliest stages of the disease before their behavior and memory begin to change.
Three trial arms were previously launched on the DIAN-TU trial platform to evaluate experimental drugs targeting amyloid. One, gantenerumab, reduced molecular markers of disease and slowed neurodegeneration in a phase 2/3 clinical trial. These promising results led the researchers to launch an exploratory open-label extension of the trial, meaning that participants in both the drug and placebo groups have been offered the drug, and the researchers continue to monitor their progress.
Although the trial focuses on people with rare mutations, drugs that are successful in this population would be promising candidates for preventing or treating the forms of Alzheimer’s that occur more commonly in older adults. The destructive molecular and cellular processes in the brain are similar in all types of the disease.







