Breast cancer prevention trial underway
Osteoporosis drug investigated in premenopausal women to see if it reduces breast density
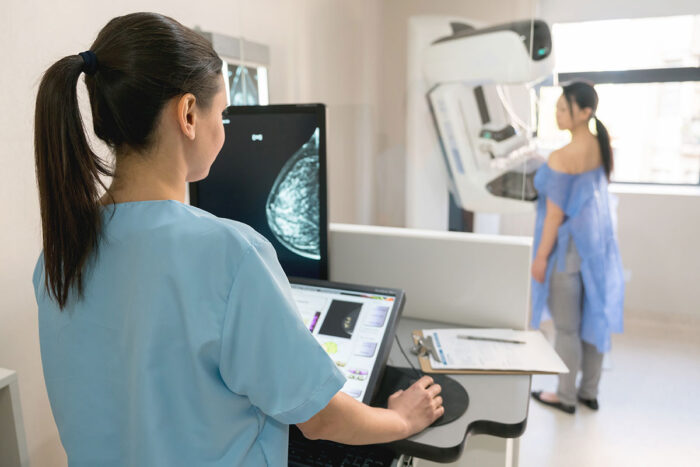 Getty Images
Getty ImagesSiteman Cancer Center and Washington University School of Medicine in St. Louis are part of a nationwide collaboration seeking to understand how the COVID-19 pandemic has affected minority and uninsured populations and their access to cancer prevention and treatment.
Some 330,000 American women are diagnosed with breast cancer each year, and researchers at Washington University School of Medicine in St. Louis are seeking ways to reduce that number.
A new $3 million grant — from the National Cancer Institute (NCI) of the National Institutes of Health (NIH) — is supporting a phase 2 clinical trial to investigate an osteoporosis drug for its potential to lower breast density in women with dense breasts. Women with dense breasts have four- to six-times higher risk of developing breast cancer than women with lower breast density. The average woman has a one in eight chance of developing breast cancer over an 80-year life span.
The trial will investigate whether the drug denosumab, approved by the Food and Drug Administration (FDA) in 2010 to treat osteoporosis, can reduce breast density in premenopausal women with dense breasts and, in the future, could be used for breast cancer prevention in these women.
“For women who have not yet gone through menopause, we do not have good preventative measures against breast cancer,” said principal investigator Adetunji T. Toriola, MD, PhD, an associate professor of surgery in the Division of Public Health Sciences. “About 25% of breast cancers are diagnosed in premenopausal women, but we have only one preventive therapy that has been approved for this group — tamoxifen, a chemotherapy drug that has undesirable side effects, including early menopause. While severe side effects are rare, tamoxifen increases a woman’s risk of developing endometrial cancer, blood clots and stroke.”
With such risks in mind, many women choose not to take tamoxifen to reduce their risk of breast cancer. Therefore, Toriola and his colleagues are seeking new preventive therapies that can reduce the risk of breast cancer with fewer undesirable side effects.
Women undergoing annual screening mammography at Siteman Cancer Center who are cancer-free and found to have dense breasts will be eligible to participate in this prevention trial. The researchers are seeking 210 participants. Trial participants must be at least 40 years old and premenopausal, and may meet any other criteria that suggest an increased risk of breast cancer, such as having a family history of the disease in a parent or sibling.
“We go through these factors in detail with the possible study participants during the screening process,” Toriola said.
The trial will not include women whose family histories of breast cancer are due to inherited mutations in the BRCA genes. Women with this genetic background and family history are at much higher risk of breast cancer, and their prevention options are different and more aggressive.
Breast density can only be assessed by having a mammogram. Dense breasts have more fibrous tissue and less fatty tissue. This trial is focused on women whose breasts show mostly fibrous or entirely fibrous tissue on a screening mammogram. About half of premenopausal women over age 40 have dense breasts. Breast density tends to decrease with age, with about 20% to 30% of women over age 70 having dense breasts.
Women with dense breasts who decide to participate in the trial will randomly be assigned to receive either the osteoporosis drug denosumab or a placebo. Denosumab is marketed under the brand names Xgeva and Prolia and has been shown to stop bone loss, thereby increasing bone density and reducing fractures associated with osteoporosis.
Denosumab blocks a molecular signaling pathway called RANK that, in addition to regulating bone remodeling, has been shown to play a role in the development of fibrous mammary gland structures as well as breast cancer in experimental models.
“The safety and effectiveness of this drug is well established in its use as an FDA-approved therapy to prevent osteoporosis and bone fractures in older women,” Toriola said. “It is given as an injection under the skin in the upper arm, upper thigh or stomach area, but it only needs to be administered every six months, rather than daily like tamoxifen. So we hope that denosumab will provide an additional prevention option for women with dense breasts who are at high risk of developing breast cancer.”
The participants will receive one dose of denosumab — or placebo — by injection at the first trial visit. Then participants will receive a second, and final, dose of either denosumab or placebo at the six-month mark. For all participants, the researchers will measure breast density by mammography at baseline and again after 12 months.
Denosumab does have side effects, including low calcium levels and muscle pain. The most severe side effect — degeneration of the jaw bone — is rare and resolves on its own when the drug is stopped, according to Toriola.
“We would like to find out if, over time, the drug has an effect on breast density and molecular markers in the breast that we know are associated with breast cancer risk,” Toriola said. “We also would like to follow these participants yearly for the following three years to see if any effects on breast density continue over a longer period of time.
“This initial phase is a five-year study,” Toriola added. “But we plan to pursue future renewals of funding in order to follow participants long enough to be able to measure whether the drug has any effect on breast cancer rates.”







