Brain, muscle cells found lurking in kidney organoids grown in lab
Researchers find simple way to prevent wayward cells from developing
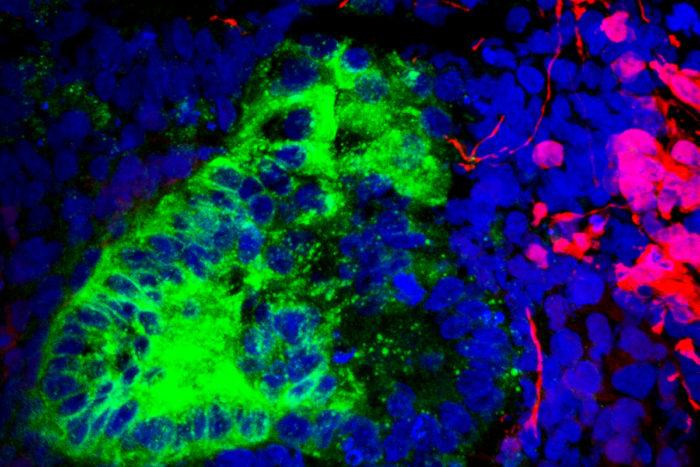 Humphreys lab
Humphreys labScientists at Washington University School of Medicine in St. Louis have identified rogue cells – namely brain and muscle cells – lurking in kidney organoids, an indication that the “recipes” used to coax stem cells into becoming kidney cells inadvertently are churning out other cell types. The researchers also demonstrated they could prevent most of those wayward cells from forming, an approach that could be adopted by scientists working with other organoids, such as those of the brain, lung or heart. The image shows brain neurons in red and kidney cells in green.
Scientists hoping to develop better treatments for kidney disease have turned their attention to growing clusters of kidney cells in the lab. One day, so-called organoids – grown from human stem cells – may help repair damaged kidneys in people or be used to test drugs developed to fight kidney disease.
But new research from Washington University School of Medicine in St. Louis has identified rogue cells – namely brain and muscle cells – lurking within kidney organoids. Such cells make up only 10 to 20 percent of an organoid’s cells, the scientists found, but their presence indicates that the “recipes” used to coax stem cells into becoming kidney cells inadvertently are churning out other cell types.
While at first glance the discovery might be viewed as a setback for using kidney organoids as stand-ins for human kidneys, there’s still promise. The researchers found an easy way to prevent most of those wayward cells from forming, and that same approach could be adopted by other scientists who find rogue cells in other organoids, such as those of the brain, lung or heart.
The research is published Nov. 15 in Cell Stem Cell.
“There’s a lot of enthusiasm for growing organoids as models for diseases that affect people,” said senior author Benjamin D. Humphreys, MD, PhD, director of the Division of Nephrology. “But scientists haven’t fully appreciated that some of the cells that make up those organoids may not mimic what we would find in people. The good news is that with a simple intervention, we could block most of the rogue cells from growing. This should really accelerate our progress in making organoids better models for human kidney disease and drug discovery, and the same technique could be applied to targeting rogue cells in other organoids.”
A major reason for the excitement around kidney organoids is the challenge of caring of patients with kidney failure. In the United States alone, nearly 500,000 people receive dialysis for end-stage kidney disease.
“Developing kidney organoids is driven by the reality that we have so many patients with failing kidneys and no effective drugs to offer them,” said Humphreys, who is also the Joseph Friedman Professor of Renal Diseases in Medicine.
For the current study, the researchers looked at two recipes widely used by scientists worldwide to grow kidney organoids. One starts with embryonic stem cells approved for research by the National Institutes of Health (NIH), and the other begins with induced pluripotent stem cells, which are reprogrammed from adult cells and have the ability to develop into any type of human cell.
A cocktail of drugs and growth factors are added to the stem cells, channeling their development into kidney cells. After growing the organoids in the lab for four weeks, a time frame long enough for the cells to specialize, the researchers asked: What kinds of cells did we get?
Rather than conduct a spot check to identify cells that made up the organoids, the researchers relied on a relatively new technique to take a deep dive. Using single cell RNA sequencing, they analyzed the activity of many thousands of genes in 83,130 cells from 65 kidney organoids.
“This generates massive amounts of data, and there’s no way our brains can make sense of it all,” Humphreys explained. “But computers can easily compare gene activity across 83,000 cells and, using artificial intelligence, group cell types together based on their gene expression. So rather than looking for cells that we think we thought we’d find in the organoid, it helped us find cells even if we’d never imagined they’d be there.”
Regardless of the recipe, the researchers found that 10 to 20 percent of the cells in the organoids missed the cue to develop into kidney cells and instead became brain and muscle cells. However, by reconstructing the step-by-step process by which stem cells developed into brain cells, for example, they were able to see precisely where things went off the rails and block the formation of off-target cells. This reduced the number of brain cells by 90 percent, and the approach provides a road map to help other scientists eliminate rogue cells in other types of organoids.
“Progress to develop better treatments for kidney disease is slow because we lack good models,” Humphreys said. “We rely on mice and rats, and they are not little humans. There are many examples of drugs that have done magically well at slowing or curing kidney disease in rodents but failed in clinical trials. So, the notion of channeling human stem cells to organize into a kidney-like structure is tremendously exciting because many of us feel that this potentially eliminates that ‘lost in translation’ aspect of going from a mouse to a human.”







