A year of COVID-19
Science, medicine rose to the occasion in the battle against the novel coronavirus, but the fight to return to normalcy rages on
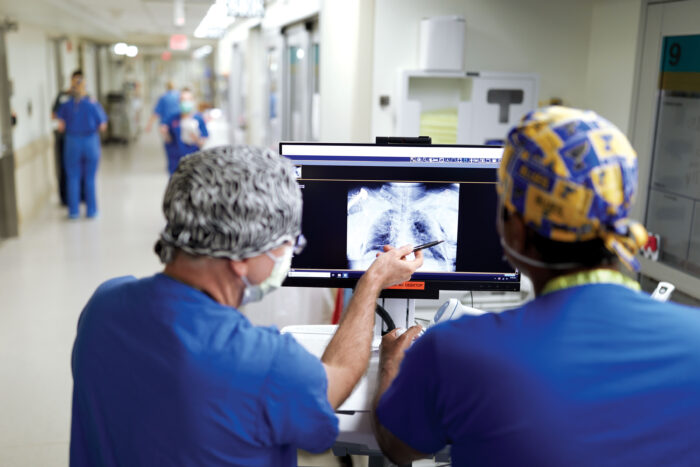 Matt Miller
Matt MillerPraveen Chenna, MD, (right) and a colleague discuss a patient's X-ray at Barnes-Jewish Hospital. Chenna is a Washington University pulmonologist who spent the past year caring for critically ill COVID-19 patients in the ICU.
A year ago this week, the World Health Organization made the alarming assessment that COVID-19 had infected people across the globe and escalated into a pandemic. Health-care workers and scientists whose work in any way touched on the highly infectious disease were called to stretch themselves like never before.
A year later, more than 2.6 million people in the world, more than 527,000 in the United States, more than 8,700 in Missouri and more than 20,000 in Illinois have died due to COVID-19. The exhausting battle to squelch the virus and address its many ramifications continues, but efforts to successfully treat the many symptoms of the disease it spurs and to develop vaccines capable of returning life to some degree of normal have been remarkable.
“We had to mobilize quickly on the Washington University Medical Campus, on multiple fronts — treating patients infected with a virus we’d never seen before, evaluating constantly evolving approaches to treatment, making sense of this virus in the lab,” said William Powderly, MD, the Larry J. Shapiro Director of the Institute for Public Health, the J. William Campbell Professor of Medicine, and co-director of the Division of Infectious Diseases at the School of Medicine, among other roles. “The teamwork and commitment to public health and to clinical and translational research I’ve seen have been tremendous. We’ve learned a great deal about this virus in the past year, with perhaps the most important lesson that we can’t let our guard down yet. We still have work to do.”
 Related: ‘It’s why we got into medicine’
Related: ‘It’s why we got into medicine’
Fierce sense of mission drives front-line workers as they treat COVID-19
Some physicians and scientists at the School of Medicine reflected on the past year and shared their thoughts on the challenges they and their colleagues and families have faced and those still to come.

Praveen Chenna, MD, a Washington University pulmonologist who has spent the past year caring for critically ill COVID-19 patients in an ICU at Barnes-Jewish Hospital.
“This experience has again reminded me why I chose this profession, why I strive to push when I feel like pulling back and why, despite the toll it has taken on health-care providers and, more importantly, patients and family members, I must push on to keep helping. I think the unrelenting pursuit to be better is what has driven us to get this far.
“The uncertainty and unpredictability of the virus impact has been unprecedented. Often, just when we thought we had an answer, it was found to be inadequate. The toll the virus has taken on daily life has been hard to imagine. Something as simple as touching our sick or dying loved ones will hopefully never be taken for granted again.
“As we work to get back to a new sense of normal, it will be important to remember that with the vaccine we must still be smart. Some of the basic safety measures such as masking, social distancing and hand washing must still be a part of our daily routine. As we begin to socialize and find an escape from the physical and mental stress that we have all endured over the past year, we must be vigilant in doing it safely.”

Tiffany M. Osborn, MD, is a critical care and emergency medicine specialist who has provided care to patients with COVID-19 over the past year.
“When the pandemic began, we did not know what we were dealing with — except that it was dangerous and deadly. Although there were good reasons to be concerned or afraid, our physicians, nurses, respiratory therapists, technicians, custodial service providers, unit secretaries, transport, admin and so many more stood shoulder to shoulder, working together to meet the needs of our community. Many suffered our own losses and milestone events within our families, yet we came to work and did our jobs with pride and compassion. I have personally witnessed the strength, compassion, humanity and, yes, beauty, in the care delivered at the bedside.
“This year has been challenging. I know we are tired for many reasons. However, we provided care and comfort to people at their most vulnerable times and made a difference in the lives of others. I am proud to walk among people who bring such value and humanity into the world.”

Virologist Michael Diamond, MD, PhD, worked with David Curiel, MD, PhD, to develop a nasal vaccine for COVID-19 that is in a phase 1 clinical trial in India. In addition, Diamond recently published research suggesting that COVID-19 antibodies and vaccines may be less effective against worrisome, rapidly spreading variants.
“In the past year, we have learned a tremendous amount about how a completely new virus causes severe disease. This has allowed us to manage it better clinically and design novel therapeutic strategies and drugs that are improving outcomes. We also learned how to make and deploy vaccines in record time. This has been nothing short of amazing.
“What’s been most challenging is the social isolation from family and friends. Working every day knowing that every experiment matters and can have an impact — this is both a blessing and a burden. Worrying about others getting sick and dying, including members of your extended family. Losing people to a disease that, if we had more time, we could control.”

Ebony Boyce Carter, MD, is an obstetrician-gynecologist who has delivered babies throughout the pandemic and whose research involves community-based interventions to promote health equity for pregnant women and their babies.
“The most challenging thing I faced in the past year was the fear early in the pandemic that, by doing the job I love, I could inadvertently be exposing my family to harm.
“I already liked my colleagues, but I love them after braving this pandemic together. We all stepped out of our comfort zone to take excellent care of patients in the face of great uncertainty and potential personal harm. We had a telemedicine system up and running in two weeks. We covered for each other without complaint through daycare closures and quarantines.
“We also felt support from others in our community — the Lowenhaupt family gave us a generous gift allowing us to give patients free blood pressure cuffs to support remote monitoring and telemedicine prenatal visits. The pandemic has shown me the very best of humanity.”

Sean Whelan, PhD, the Marvin A. Brennecke Distinguished Professor and head of the Department of Molecular Microbiology, transformed an unused room in his lab into a biosafety level 3 (BSL-3) laboratory in a matter of weeks so that he could study the SARS-CoV-2 virus. As part of his research, he developed a hybrid virus that infects cells and is recognized by antibodies but lacks the ability to cause severe disease. The hybrid virus made it possible for researchers across the world to study COVID-19 under normal laboratory conditions.
“We’ve learned that infectious diseases — particularly emerging infectious and drug-resistant microbes — pose a serious threat to our society for which we need to be better prepared. Looking ahead, we’ll need to develop a national strategy to coordinate research and plan how to respond to future pandemics.
“It’s been challenging to see the undermining of experts in science and public health, as well as the politicization of science and the public health measures (such as wearing masks and social distancing) to combat the pandemic.”

Steven Lawrence, MD, is an infectious disease expert who studies how to better understand the natural history, impact and mitigation of potentially large-scale infectious disease outbreaks.
“Having millions of doses of three fully tested, safe and effective vaccines within 12 months of a pandemic virus first being identified is mind-boggling. And over the past year, we have learned that human connection is precious and dearly missed when it is taken away; rational decision-making based on scientific evidence is difficult during a pandemic and that we often make decisions based on emotion; and systemic racism is real and can have direct large-scale detrimental effects on health.
“Most challenging in the past year has been watching a mounting death toll in the face of reluctance to consistently message and model the behaviors that would have averted many deaths. A major challenge in the next six months will be navigating how to emerge from the pandemic safely. Some will ditch mitigation measures too quickly and others will cling to them for psychological safety beyond the duration they are needed. How do we factor into the reality that vaccinated individuals have less, but not zero, risk when not everybody has yet had a chance to be vaccinated? How will requiring proof of vaccination further lead to inequities?”

Elvin Geng, MD, is an epidemiologist and an infectious diseases physician. During the pandemic, he helped develop a platform to track information about local transmission that officials have needed to make public health decisions.
“We’ve learned that it is entirely possible to not only flatten the curve but end the pandemic through modifying behavior. But you have to have the right mobilization and social and economic fabric to do so – and we did not.
“The fact that this epidemic may not come to a close, with emergent COVID variants circulating, is something we may have to live with forever. The world will have a hard time accepting that.”

Jessica Gold, MD, is a psychiatrist who has focused on treating Washington University health-care workers, employees and family members during the pandemic.
“When I think about COVID one year later, it is amazing to think it has been a year since all of our jobs, lives, work lives, have been upended. I think about how mental health permeates every conversation. When we have uncertainty, we have anxiety. When we have social isolation, we have loneliness and depression. When we have loss, grief, job loss, transition, or are health-care workers on the front lines, it can cause sustained trauma. I think it is important to say that out loud, so we can start processing and coping with it.
“We have learned that connection matters — even the smallest connection. We took for granted how much we liked seeing each other, even in the office, and that even the most introverted among us like to have places where we bump into peers. We like structure, and the change and work/life blend has been hard for all of us. We have had to institute a lot of our own structure on top of all we’re dealing with, to help our mental health.
“Mental health challenges come later — even years later — when people assess the damage and we do not have enough resources to handle the mental health challenges that will stem from the pandemic. We will see long wait lists for care and people who don’t get care. This will be an ongoing issue, and I am not sure how we will manage it.”
For more details on how the Medical Campus has responded to the pandemic, see here.







