$5 million grant endows research to advance blood disorder therapies
Edward P. Evans Foundation funds new center focused on myelodysplastic syndromes
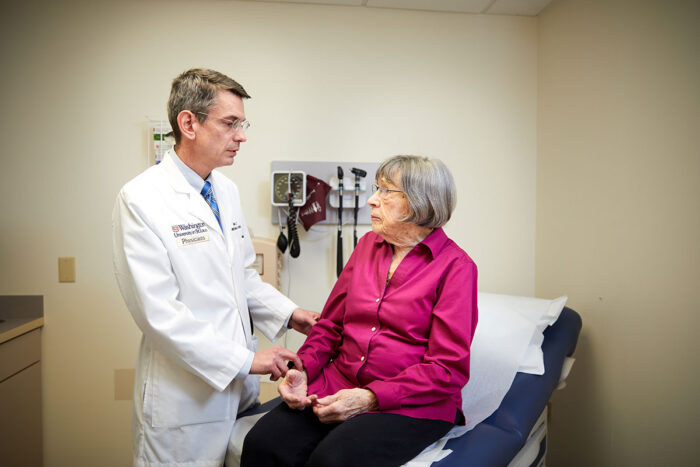 Matt Miller
Matt MillerMatthew Walter, MD, (left) speaks with Gloria Berkman, a patient with myelodysplastic syndrome (MDS), a rare blood disorder that prevents the body from making enough healthy blood cells. Walter is leading a new center focused on MDS research and patient care at Washington University School of Medicine in St. Louis.
Washington University School of Medicine in St. Louis has received a $5 million grant from the Edward P. Evans Foundation to establish and endow a new center focused on advancing research and improving treatments for a rare set of blood disorders called myelodysplastic syndromes, or MDS, that leaves the body unable to make enough healthy blood cells.
The new Edward P. Evans Center for Myelodysplastic Syndromes at Washington University will be led by oncologist Matthew J. Walter, MD, a professor of medicine who treats patients with MDS and related blood disorders at Siteman Cancer Center at Barnes-Jewish Hospital and Washington University School of Medicine.
Difficult to diagnose, MDS is characterized by low blood cell counts. Symptoms can be vague, such as fatigue and shortness of breath. It can be fatal, but people with low-risk MDS may live for years with the disease and never realize they have it. Patients are diagnosed based on the appearance of their abnormal blood cells, and doctors often take a watchful waiting approach to see if their blood cell counts decrease or the number of abnormal blood cells increases before taking steps to intervene. In about one-third of MDS patients, the slow-growing disease takes an aggressive turn and progresses to acute myeloid leukemia (AML), a fast-growing cancer of the blood that is fatal unless successfully treated with a stem cell transplant. Even so, long-term prognosis for almost all AML patients is poor. About 40,000 people are diagnosed with MDS in the U.S. each year.
“The only way to cure MDS is a stem cell transplant,” Walter said. “And patients with MDS are usually older, say in their 70s, when it is much harder for the body to tolerate such a transplant. So we can treat the disease in older patients with chemotherapy and blood transfusions, but we have no way to cure it in people who aren’t candidates for a stem cell transplant. We want to study how MDS occurs so we can intervene and prevent it from progressing.”
Walter and his colleagues are interested in identifying healthy individuals with normal blood counts and mutations in a few key genes that are linked to MDS but who don’t have any symptoms. This condition is called age-related clonal hematopoiesis (ARCH). Individuals with ARCH have a higher than average but still relatively low risk of developing MDS — about 1% per year, as well as a higher risk of developing other age-related conditions, such as cardiovascular disease. Although relatively few will end up with MDS, studying this group of patients could help doctors understand the differences between those patients who go on to develop disease and those who don’t.
A major goal of the center is to launch an ARCH clinic that will see patients and conduct a long-term study tracking the courses of their disease. The researchers estimate that about 10% of 70-year-olds have ARCH.
According to Walter, almost all ARCH patients — about 95% — who go on to develop low blood counts will be diagnosed with MDS or leukemia sometime over the next 10 years. This suggests that ARCH may be a precursor to MDS. But why one person develops MDS and another doesn’t remains a mystery.
“We have a chance to understand the genetic factors or the environmental factors that might tip the balance, leading patients to develop MDS,” Walter said. “It’s a challenge to identify patients with ARCH because they are healthy. They have normal blood counts with just a very small number of abnormal cells. So we have to use genetic sequencing data to find people with mutations in certain genes that we know are involved in MDS and AML.”
Environmental risk factors for MDS include previous chemotherapy and radiation to treat other cancers as well as exposure to benzene or radiation on the job, for example. The researchers affiliated with the center would like to learn more about environmental stresses that could interact with gene mutations and drive the disease to progress. The goal would be to find ways to reduce those stresses and thereby reduce the risk of worsening the condition.
The center also will have the ability to collect and store blood samples for genetic analysis. The researchers ultimately would like to develop prevention strategies to stop ARCH from progressing to MDS. Walter and his colleagues also would like to develop new immunotherapies and new strategies for stem cell transplantation that might be less toxic than traditional approaches to treating MDS.
Currently, 16 investigators from oncology, cardiology and the McDonnell Genome Institute at Washington University are participating in the center. The center will foster collaborations between established MDS researchers and those new to the field and provide research funding for innovative projects. Its endowment also will support a fellowship for researchers-in-training and a professorship, both named for Edward P. Evans.
In addition to major support from the Department of Medicine and Siteman Cancer Center, the new center is positioned to benefit from other major initiatives supporting leukemia research at the School of Medicine, including the Genomics of Acute Myeloid Leukemia (AML) Program Project Grant led by Timothy J. Ley, MD, the Lewis T. and Rosalind B. Apple Professor of Medicine, and the Specialized Program of Research Excellence (SPORE) grant in leukemia led by Daniel C. Link, MD, the Alan A. and Edith L. Wolff Professor of Medicine. Those initiatives are funded by the National Cancer Institute of the National Institutes of Health (NIH). In addition, the center will benefit from the long-standing collaboration between MDS researchers and the McDonnell Genome Institute. Such resources make Washington University a national hub for innovative research and leadership in developing new therapies for patients with cancerous blood disorders.
Edward Parker Evans was a businessman, philanthropist and horseman. His Spring Hill Farm in Casanova, Virginia, was the largest thoroughbred breeding farm in the state. Evans established his foundation in 1984. Since his death from secondary acute myelogenous leukemia in 2010, the Edward P. Evans Foundation has supported collaborative and transformational research on MDS at leading institutions. Washington University will be hosting the EvansMDS Summit on Oct. 24 and 25, where investigators working on the most groundbreaking MDS research will present their research.
“The Edward P. Evans Foundation has contributed more than $66 million since 2011 to medical research directed at improving outcomes and finding a cure for MDS patients,” said Michael D. Lewis, PhD, president of the foundation. “Washington University is an ideal location for our first Edward P. Evans Center for Myelodysplastic Syndromes. The center capitalizes on an array of world-renowned faculty and the resources of the Siteman Cancer Center and McDonnell Genome Institute. We eagerly anticipate the flow of new discoveries that will benefit MDS patients.”







