Studying the effects of traumatic brain injury in war zones
Early psychological symptoms may be a predictor of later disability in military personnel with mild concussions
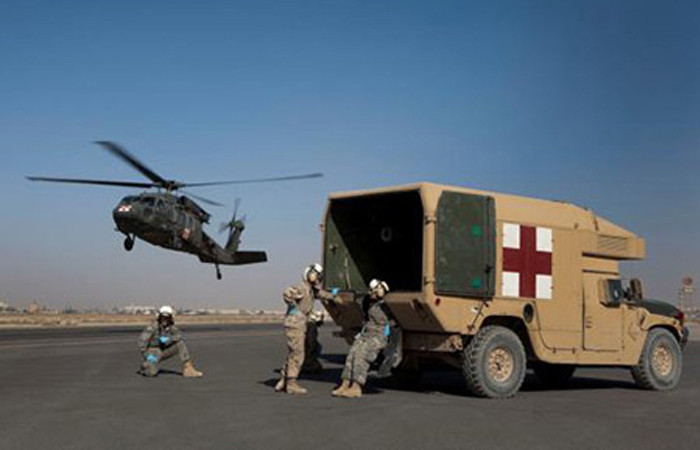 Octavian Adam
Octavian AdamA U.S. military helicopter in Afghanistan meets with service members for a medical evacuation. New research led by Washington University School of Medicine finds that when evaluating military personnel with mild traumatic brain injuries, early symptoms of post-traumatic stress are the strongest predictors of later disability.
When doctors evaluate military personnel with blast-related mild traumatic brain injuries, they generally test for things like memory, thinking, balance, coordination and severity of headaches and dizziness. But according to a new study led by Washington University School of Medicine, stronger predictors of later disability include early mental health symptoms of post-traumatic stress, such as anxiety, emotional numbness, flashbacks and irritability.
“Symptoms of post-traumatic stress and depression have always been thought to develop months to years later,” said David L. Brody, MD, PhD, a Washington University neurologist at Barnes-Jewish Hospital. “We don’t know what causes these symptoms, whether they result from the brain injury itself, from the stress of war or some combination of factors. But regardless of their origin, the severity of these psychological symptoms soon after injury was the strongest predictor of later disability.”
The study also suggests that mild concussions have more severe long-term effects than previously thought, including difficulty returning to previous work, family and social activities. The results raise questions about how best to treat U.S. troops who suffer head injuries.
During the conflicts in Iraq and Afghanistan, about one-fifth of service members experienced a head injury, according to recent estimates from the U.S. Department of Defense, and more than 80 percent of those were considered mild.
The research, which was done in partnership with the U.S. military, investigators at Washington University in St. Louis and the Naval Medical Center Portsmouth in Virginia, evaluated traumatic brain injury from blast exposure in active-duty military personnel stationed in Afghanistan in 2012.
The study is the first to evaluate active-duty service members with blast-related mild concussions very early, in the first week after injury. The researchers used standard military mental health questionnaires to assess symptoms of post-traumatic stress disorder, such as experiencing repeated, disturbing memories or dreams, feelings of emotional numbness, difficulty concentrating and feelings of anger or hyper-alertness. They then combined that data with follow-up mental health evaluations of the same patients 6-12 months later. Most other studies of traumatic brain injury in military personnel have focused on those who are more severely injured and have been evacuated from war zones.
Psychological evaluations after brain injury
The findings suggest that care for military personnel with brain injuries should be broadened to include psychological evaluations earlier in the process. The same criteria are used to decide when civilians should return to sports, school or work after concussions, and whether a service member should return to active duty. These criteria are currently focused on cognitive function and clinical symptoms and do not include assessments of mental health.
Brody and his colleagues are planning a similar study of civilian concussions, looking at mental health measures immediately following mild head injuries in patients who come to the emergency room. Those patients will be followed to determine long-term outcomes.
“The lessons that we learn from military trauma apply quite readily to civilian trauma,” Brody said. “Still, there may be unique aspects of military brain injury that are not true in the civilian world. It could also be that this is a general phenomenon that has not been carefully addressed in civilian or military populations.”
Read the full story in the newsroom.








