Simulator aids video-assisted lung cancer surgery training
A novel simulator is helping surgeons learn to perform video-assisted thoracoscopic surgery (VATS) on patients with lung cancer
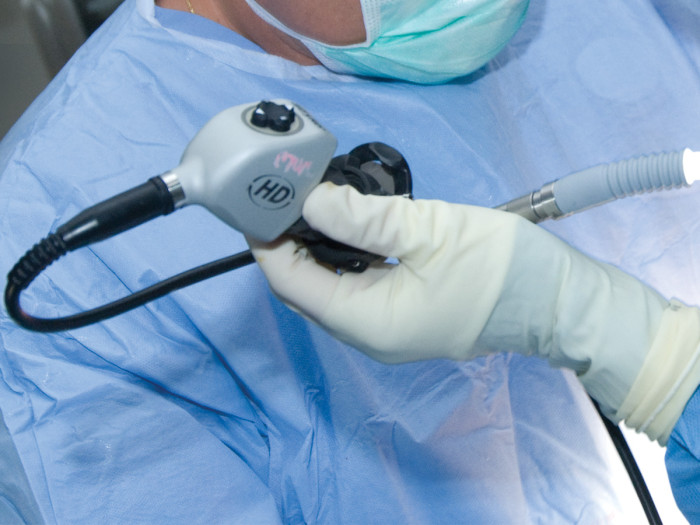
A surgeon performs video-assisted thoracoscopic surgery (VATS).
Video-assisted thoracoscopic surgery (VATS) is a minimally invasive lung surgery procedure in which a section of lung is removed through a series of tiny incisions rather than a large incision that involves cutting through muscle and spreading the ribs. Tiny cameras inserted through the incisions transmit images onto a video monitor that the surgeon views throughout the procedure.
“VATS results in less pain and a shorter length of stay for the patient without compromising the results,” says Washington University cardiothoracic surgeon Traves Crabtree, MD, who invented the simulator. “The problem is that it’s a technically more challenging operation to teach and learn than traditional open surgery, so getting surgeons on board has been a challenge.”
Developing a life-like model
Crabtree, who teaches in the bioengineering program and at the School of Medicine, came up with a solution. Known as the Crabtree VATS Simulator, the synthetic, mannequin-like device is an anatomically accurate model of one side of the chest called hemithorax – with lung, heart, ribs and diaphragm all included – that has lifelike bone structure, musculature, soft tissue and skin. The model also circulates fluid through the blood vessels to simulate blood flow and mimic human blood pressures. Crabtree based his design on computer models generated from human computed tomography scans.

Another advantage of the simulator is that surgeons don’t have to travel to another location to train.
“Surgeons will be able to practice with the simulator in their own operating environment, with their own assistants and their own equipment. They can use it repetitively to learn how to perform the procedure,” says Crabtree, who previously invented a percutaneous device to repair the mitral valve.
The VATS simulator is patent-pending, and Ethicon Inc. purchased a few models for use in a training course in Las Vegas in early 2015. Based on feedback from surgeons who took the course, Crabtree is making adjustments to the simulator.
“This simulator should decrease the learning curve for surgeons,” Crabtree says. “They can use it as much as necessary before putting what they’ve learned into practice.”
Crabtree is a paid consultant for Ethicon.








